The Panic After Stopping the Pill
A friend texted me in a panic: "I've been on the pill for 8 years. I'm coming off to try for a baby, but my mum says I've probably damaged my fertility. She thinks I should have come off ages ago to 'let my body recover.' Now I'm terrified I've left it too long."
I've heard versions of this worry countless times. "The pill ruins your fertility." "You need to wait months after stopping before trying." "IUDs cause infertility." "The longer you're on birth control, the harder it is to conceive."
These myths are everywhere, and they're causing unnecessary anxiety for couples trying to conceive. Worse, these fears prevent some people from using highly effective contraception in the first place.
So let's look at what the research actually says about birth control and fertility—because the truth is far more reassuring than the myths.
Myth #1: "The Pill Damages Your Fertility"
The Claim: Years of hormonal contraception have "shut down" your reproductive system and made it harder (or impossible) to get pregnant.
What the Research Shows:
A comprehensive 2018 systematic review and meta-analysis looked at contraceptive discontinuation and return to fertility. The findings:
- 83.1% of women became pregnant within 12 months of stopping contraception
- This rate was the same regardless of contraceptive method (pills, IUDs, implants)
- Duration of contraceptive use did NOT affect fertility
- The type of progesterone in birth control did NOT affect fertility
The researchers concluded: "Contraceptive use regardless of its duration and type does not have a negative effect on the ability of women to conceive following termination of use and it doesn't significantly delay fertility."
How Quickly Does Fertility Return?
A Boston University study of 17,954 women found average time to fertility return varied by method:
- IUDs and implants: 2 menstrual cycles
- Birth control pills and vaginal rings: 3 cycles
- Patch: 4 cycles
- Injectable contraceptives (Depo-Provera): 5-8 cycles
Within 12 months of stopping any method, 77% of women had conceived.
The pill's hormones leave your body within a week of stopping. Most women resume ovulating within 1-2 months.

What About "Post-Pill Amenorrhea"?
In the 1960s-70s, high-dose birth control pills were linked to delayed return of periods after stopping. This created lasting fears about the pill damaging fertility.
But modern low-dose pills don't cause this. Research since the 1990s has shown that women who experienced irregular periods after stopping the pill typically had menstrual irregularities BEFORE starting—the pill just masked them.
The Bottom Line:
The pill does not damage your fertility. Duration of use doesn't matter. You don't need to "let your body recover" before trying to conceive.
Myth #2: "IUDs Cause Infertility"
The Claim: Having an IUD (especially for years) damages your uterus or tubes, making it harder or impossible to get pregnant later.
What the Research Shows:
Copper IUDs
A New Zealand study followed 887 women who had copper IUDs removed to conceive:
- 94% became pregnant within 36 months
- Duration of IUD use (less than 2 years vs 2+ years) did NOT affect fertility
- No increased risk of ectopic pregnancy compared to other methods
A UT Southwestern study found 87% of women who had IUDs removed became pregnant within one year.
Hormonal IUDs
Hormonal IUDs (like Mirena) release small amounts of progest into the uterus—not systemically like the pill. Once removed:
- Fertility returns within 1-2 months for most women
- No lasting effect on ovulation or fertility
- No increased risk of complications
Copper vs Hormonal: Copper IUDs don't use hormones, so fertility can return immediately upon removal. Hormonal IUDs may take a week or two for your cycle to resume, but there's no long-term impact either way.

The Historical Confusion
Fears about IUDs and fertility stem from the Dalkon Shield disaster in the 1970s. This particular IUD was linked to pelvic infections and infertility, and was pulled from the market.
Modern IUDs are completely different devices with excellent safety profiles. They don't cause infertility.
The Bottom Line:
IUDs (copper or hormonal) do not cause infertility. You can get pregnant as soon as they're removed—sometimes within days for copper IUDs.
Myth #3: "You Need to Wait Months After Stopping Birth Control Before Trying"
The Claim: You must wait 3-6 months after stopping the pill or removing an IUD to "flush out" hormones or "let your body recover" before trying to conceive.
What the Research Shows:
This is outdated advice from the 1970s-80s when people feared higher miscarriage risks if you conceived immediately after stopping high-dose pills.
Modern research shows:
- No increased miscarriage risk if you conceive immediately after stopping contraception
- No need to wait before trying to conceive
- Pill hormones clear your system within a week
The ONLY reason doctors sometimes suggest waiting is practical: it makes it easier to date the pregnancy accurately if you've had at least one natural period. But medically, you can start trying immediately.
Exception: Depo-Provera (Injectable)
The injectable contraceptive is different. It delivers a large dose of progestin meant to last 12-13 weeks. After your last shot:
- Some women resume ovulating within 3 months
- Others can take up to 18 months (occasionally longer)
- But eventual fertility rates are the same as other methods
If you know you want to conceive in the near future, Depo might not be the best choice—not because it damages fertility, but because it takes longer to clear your system.

Myth #4: "The Longer You're On Birth Control, The Worse It Is"
The Claim: Every year you spend on hormonal contraception further damages your fertility. If you've been on it for 5-10 years, you've done serious harm.
What the Research Shows:
The 2018 meta-analysis specifically examined this and found: "Duration of oral-contraceptive use do not significantly influence the return of fertility following cessation of contraception."
Studies comparing women who used contraception for:
- Less than 2 years
- 2-5 years
- 5-10 years
- 10+ years
Found NO significant differences in time to pregnancy after stopping.
A Human Reproduction study confirmed: "Previous use of oral contraceptives did not impair fertility."
Why This Myth Persists:
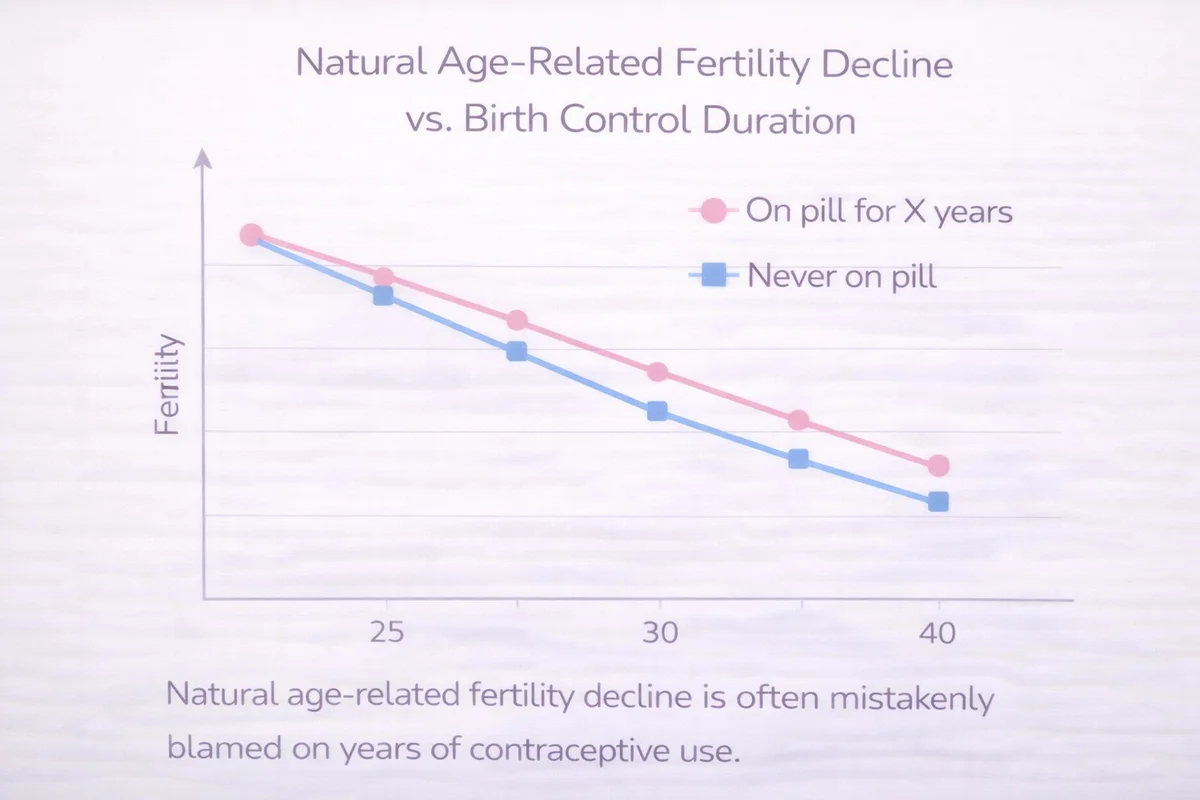
Age. Women who've been on the pill for 10 years are 10 years older than when they started. Fertility naturally declines with age—particularly after 35. The pill didn't cause the decline; aging did.
If you started the pill at 25 and stop at 35, you're less fertile than you were at 25. But you're no less fertile than a woman who never used birth control and is now 35.
The Bottom Line:
Duration of contraceptive use doesn't affect fertility. Use it as long as you need it—when you stop, fertility returns regardless of how many years you were on it.
What Birth Control CAN Do (And Why That Matters)
While birth control doesn't cause infertility, it can mask underlying conditions that affect fertility. This is important to understand:
Birth Control Can Hide:
- Irregular cycles: The pill regulates periods, so you won't know if you have irregular ovulation
- PCOS symptoms: Birth control treats PCOS symptoms (irregular periods, acne, excess hair)
- Endometriosis: Hormonal contraception reduces endometriosis pain
When you stop birth control to try to conceive, these underlying conditions become apparent. The birth control didn't cause them—it just covered them up.
Example:
Sarah was on the pill for 8 years. When she stopped, her periods didn't return regularly. After 6 months, she was diagnosed with PCOS.
Did the pill cause her PCOS? No. She likely had it before starting the pill (which is why her periods were irregular then too). The pill masked her PCOS symptoms for 8 years. When she stopped, the PCOS symptoms returned.
This is actually one argument FOR earlier diagnosis—but the pill itself didn't cause the condition.
When To Actually Worry
If you've stopped birth control and:
- Haven't had a period in 3-4 months (and you're not pregnant)
- Trying for 12 months without success (if you're under 35)
- Trying for 6 months without success (if you're 35+)
See your GP. But the issue won't be the birth control—it's something else that needs investigation.
The Real Fertility Factors
If you're concerned about fertility, focus on factors that actually matter:
What DOES Affect Fertility:
- Age (biggest factor—declines significantly after 35)
- Smoking (reduces fertility in both partners)
- Weight (significantly overweight or underweight)
- STIs (untreated chlamydia/gonorrhea can damage tubes)
- Medical conditions (PCOS, endometriosis, thyroid disorders)
- Male factor issues (50% of infertility involves male factors)
What DOESN'T Affect Future Fertility:
- Years on the pill
- Duration of IUD use
- Number of times you've switched birth control methods
- Taking the pill continuously (skipping periods)
- Using the morning-after pill
The Real Story
I mentioned my friend who panicked about 8 years on the pill. Here's what happened:
She stopped the pill. Had her first natural period 5 weeks later. Started trying to conceive immediately. Got pregnant on cycle 3.
Her 8 years on the pill had zero impact on her fertility.
The irony? Her mum's generation used high-dose pills with more side effects, which fueled these myths. Modern low-dose contraception is completely different. But the outdated fears persist.
When she told her mum she was pregnant, her mum said: "See? Your body just needed time to recover from all those years on the pill!"
No. Her body just needed to ovulate and for sperm to meet egg. The pill had nothing to do with how long it took.
The Bottom Line
- Birth control pills do NOT damage fertility, regardless of duration of use
- IUDs (copper or hormonal) do NOT cause infertility
- You do NOT need to wait months after stopping before trying to conceive
- Fertility returns quickly for most methods (except Depo can take longer)
- 83% of women conceive within 12 months of stopping any contraceptive method
- If you're struggling to conceive, the birth control isn't the cause
Use whatever contraception works best for you, for as long as you need it. When you're ready to try for a baby, stop the method and start trying. Your fertility will be exactly what it would have been if you'd never used birth control in the first place—plus or minus natural age-related changes.
Disclaimer: This information is based on peer-reviewed studies and medical guidance, but isn't medical advice. If you have concerns about contraception or fertility, speak to your GP or a family planning specialist.




