The Panic After the First Negative Test
After our third month of negative pregnancy tests, I started Googling. Mistake.
Within minutes, I'd convinced myself my running habit was the problem. I'd been running 25-30 miles a week for years. Surely that was "too much." I should stop immediately, right?
But then I found an article saying sedentary women have lower fertility rates. So maybe I should run more?
Then another claiming marathon training caused infertility. But wait—plenty of elite athletes get pregnant mid-season.
I felt paralysed. Was I harming my chances every time I laced up my trainers? Or would stopping exercise make things worse?
The answer, frustratingly, is: it depends.
Let's sort through the exercise and fertility myths—because the truth is far more nuanced (and reassuring) than the internet would have you believe.
Myth #1: "You Need to Stop All Exercise When TTC"
The Claim: Any vigorous exercise while trying to conceive will harm your fertility. You should switch to gentle yoga or walking only.
What the Research Shows:
This is categorically false for most women.
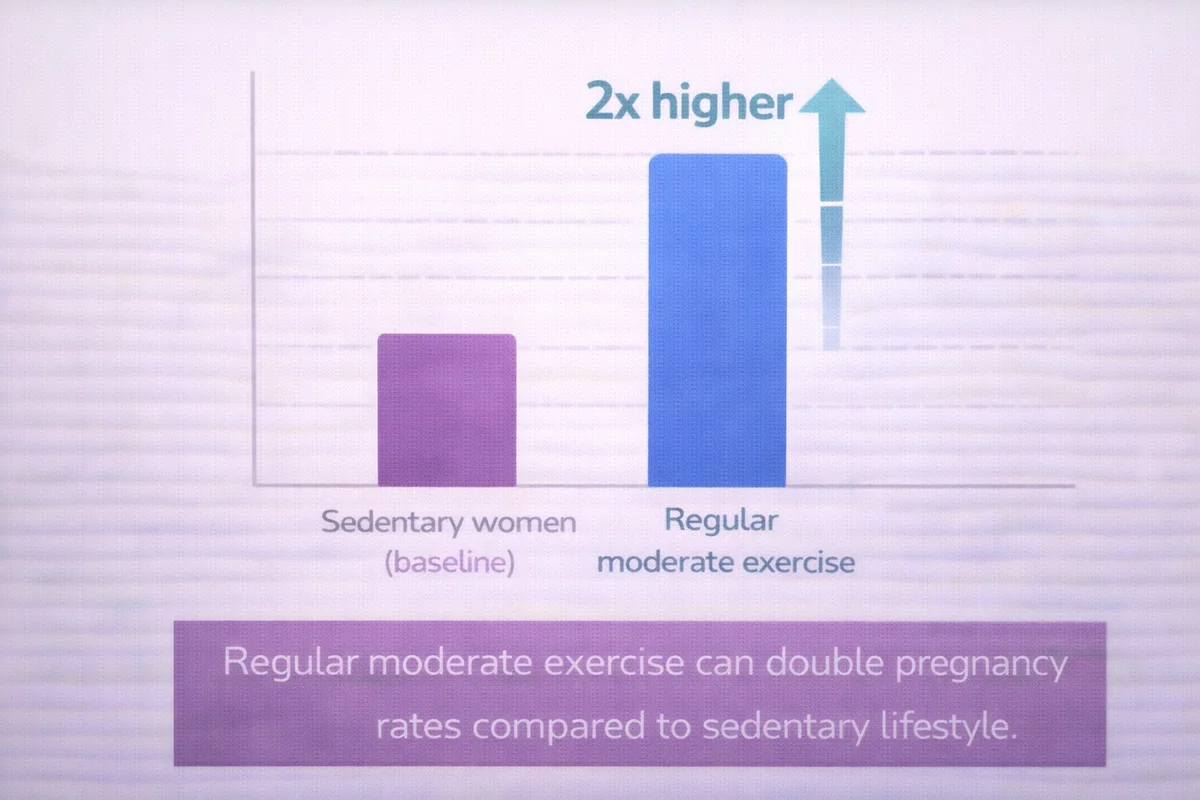
A 2019 meta-analysis (combining data from multiple studies) found that pregnancy rates can be TWICE as high in women maintaining regular exercise compared to sedentary women.
A large study found:
- 2 hours of moderate exercise per week increased pregnancy odds by 15%
- Regular exercise benefits fertility through mechanisms other than weight loss
- Even women at healthy weights benefit from regular physical activity
Why Exercise Helps Fertility
Research shows regular exercise:
- Regulates hormones (estrogen, progesterone, testosterone, insulin)
- Improves insulin sensitivity (crucial for ovulation)
- Reduces stress and cortisol levels
- Maintains healthy body weight and BMI
- Improves blood flow and circulation
For women with PCOS or obesity, exercise is especially beneficial and actively recommended.
The Bottom Line:
"The number one recommendation is to assume you're fertile unless proven otherwise," says Alice Domar, director of the Domar Center at Boston IVF. "If you are a runner and you have regular menstrual cycles, I wouldn't worry about changing your routine unless you can't get pregnant."
Myth #2: "More Exercise Is Always Better"
The Claim: If moderate exercise helps fertility, then more exercise must help even more. Train harder, run longer, push yourself.
What the Research Shows:
Not quite. There's a tipping point where too much vigorous exercise can harm fertility.
A major study found:
- Women exercising 5+ hours per week of vigorous exercise were 32% less likely to conceive
- Women exercising 3-4 hours per week of vigorous exercise were 27% less likely to conceive
- But 2 hours of moderate activity increased pregnancy odds by 15%
Another study found women categorized as "high" physical activity index were 1.5 times more likely to experience subfertility compared to women with "low" activity.
But Here's the Critical Finding...
A 2015 randomised controlled trial revealed the KEY factor isn't the exercise itself—it's energy deficit.
Researchers put athletes into energy deficits of 15%, 30%, or 60% while maintaining exercise:
- ALL groups with energy deficit had menstrual cycle issues
- Anovulation (not releasing an egg)
- Shorter luteal phase
- Lower progesterone
The control group with appropriate energy balance had normal cycles—despite exercising the same amount.

What This Means for Athletes
Researchers concluded: "Women wanting to continue their vigorous exercise regimen while attempting to conceive could be instructed to ensure that on workout days, they increase their caloric intake by approximately the number of calories expended during their exercise session."
The Bottom Line:
Vigorous exercise CAN harm fertility—but only when combined with inadequate calorie intake. If you're eating enough to match your energy output, you can likely continue high-intensity training.
Myth #3: "There's a Specific Mileage/Hours Limit"
The Claim: Don't run more than X miles per week, or don't exercise more than Y hours per week when TTC.
What the Research Shows:
There's no universal threshold because every woman is different.
"The reason for the lack of specific mileage guidelines is that every woman is different," explains Dr. Sarah Crane, OB/GYN at Boston University. "Some get pregnant in the middle of marathon training; for others 20-mile weeks may be too much."
Why Individual Variation Matters
Factors that determine YOUR threshold:
- Current body weight and BMI
- Calorie intake vs expenditure
- Training history and adaptation
- Menstrual cycle regularity
- Stress levels
- Sleep quality
- Overall health
A woman with higher body fat percentage and regular periods might handle 50+ mile weeks fine. A lean runner with borderline BMI might need to cut back to 20 miles.
The Bottom Line:
Don't fixate on arbitrary numbers. Monitor your menstrual cycle—that's your best indicator of whether your exercise level is appropriate.
The One Reliable Indicator: Your Menstrual Cycle
Here's the most important thing: If you have regular periods, your exercise level is probably fine.
What "Regular" Means
For women aged 18-35, a normal cycle is 22-33 days long consistently.
Red Flags to Watch For
Signs your exercise might be affecting fertility:
- Irregular cycles (varying more than a few days month to month)
- Amenorrhea (no period for 3+ months)
- Very long cycles (35+ days consistently)
- Anovulatory cycles (you're bleeding but not ovulating)
- Unrelenting fatigue that doesn't improve with rest
- Persistent soreness and poor recovery
After Stopping Hormonal Birth Control
It can take up to 3 months for your cycle to regulate after stopping the pill or other hormonal contraception. If cycles are still abnormal after 3 months, evaluate your exercise and nutrition.

The Bottom Line:
Regular periods = green light to continue your current exercise routine. Irregular or absent periods = time to reassess.
When Exercise Helps Fertility: PCOS and Obesity
For some women, more exercise is actually the prescription.
Women with PCOS
Polycystic ovary syndrome (PCOS) affects 1 in 10 women and is a leading cause of infertility.
- Exercise improves insulin sensitivity (crucial for PCOS)
- Benefits appear after about 50 training hours (roughly 1 month of moderate-vigorous exercise)
- Exercise improves fertility even without weight loss
- Healthy-weight women with PCOS also benefit from vigorous exercise
Women with Obesity
For women with BMI over 30, exercise is actively encouraged.
A study of 216 obese women undergoing IVF found:
- 39% success rate for women who exercised regularly
- 16% success rate for sedentary women
- Live birth rates: 24.4% vs 7.4%
Studies show improved cycle regularity, ovulation, and live births in obese women who increase exercise—even when the number on the scale doesn't change.
The Bottom Line:
If you have PCOS or obesity, exercise is your friend. Don't hold back—consistent moderate-to-vigorous exercise can significantly improve your fertility.
When Exercise Might Harm Fertility: Low BMI and Energy Deficit
There's a flip side: some women need to reduce exercise or increase calories.
Who Should Consider Cutting Back
- Your BMI is below 20 (or low-normal, around 20-21)
- You have irregular or absent periods
- You're not ovulating regularly
- You have diagnosed functional hypothalamic amenorrhea
- You're experiencing signs of overtraining
The BMI Caveat
"Although underweight is defined by a BMI of 18.5," explains Dr. Crane, "some women with BMIs at the lower end of normal (in the low 20s) may need to gain a few pounds before they can conceive."
Real-World Example
Jennifer Fox, a marathoner, had a normal BMI but abnormally long cycles. She wasn't ovulating, and fertility medications didn't help.
Her doctor advised cutting back running. "I was frustrated because that was a source of joy for me," Fox said. But after gaining just 5 pounds and slightly reducing mileage, she started cycling again and eventually conceived.
The Bottom Line:
"In order to get pregnant, your body has to believe that it's a good time for you to build a baby… that you are in a relatively safe place with enough calories to support a pregnancy," says Dr. Domar.
Exercise and Male Fertility
Let's not forget the other half of the equation.
Exercise Helps Men Too
Studies show men who engage in vigorous exercise 15+ hours per week have:
- Higher sperm concentrations
- Higher total sperm counts
- Better overall sperm quality
Compared to sedentary men.
Research consistently finds men who exercise regularly have better sperm quality and higher pregnancy rates with their partners.
Benefits for Men
Regular exercise:
- Boosts testosterone levels
- Improves sperm motility and morphology
- Helps maintain healthy weight
- Reduces stress
The Bottom Line:
For men trying to conceive, regular exercise is beneficial. Unlike women, there's less concern about "too much" exercise harming male fertility (though extreme overtraining can affect testosterone).
Practical Guidelines: What Actually Works
So what should you actually DO?
If You Have Regular Periods (22-33 Days)
Continue your current exercise routine. Regular periods indicate your body has adequate energy to support reproduction. Don't change anything unless you've been trying for 12 months (or 6 months if 35+) without success.
If You're Sedentary
Start exercising. Aim for:
- 150 minutes of moderate-intensity activity per week (brisk walking, swimming, cycling)
- Or 75 minutes of vigorous activity (running, HIIT, competitive sports)
- Or a combination
This can improve your fertility by 15% and supports overall health.
If You Exercise 5+ Hours/Week Vigorously
Check your menstrual cycle:
- Regular periods? You're fine—just ensure adequate calorie intake
- Irregular/absent periods? Either:
- Increase calorie intake to match energy expenditure, OR
- Reduce vigorous sessions to 1-2 per week, with other sessions moderate intensity
If You Have PCOS or Obesity
Increase exercise to moderate-vigorous intensity:
- Aim for at least 150 minutes per week
- Include both cardio and strength training
- Don't worry if weight doesn't change—exercise benefits fertility through other mechanisms
If You Have Low BMI or Irregular Cycles
Consider adjusting:
- Increase calorie intake first
- Gain 3-5 pounds if BMI is low-normal
- Reduce vigorous exercise to 1-2 sessions per week
- Focus on moderate-intensity activities
- Monitor whether cycles normalize within 2-3 months

What Happened With Me
Remember my panic about running 25-30 miles per week?
I had regular 28-day cycles. I was at a healthy BMI (22). I was eating well.
So I kept running. And conceived on month 4—which is completely normal and has nothing to do with my mileage.
The key? I was paying attention to my body:
- Regular periods: check
- Good energy: check
- Adequate calories: check
- No signs of overtraining: check
My running wasn't the problem. Impatience was.
The Research Bottom Line
According to Dr. Lora Shahine, reproductive endocrinologist: "Those who love running shouldn't have to give it up while trying to conceive." But modifications to intensity or duration are worth considering if you have irregular cycles or low BMI.
The evidence shows:
- Moderate exercise improves fertility (by about 15%)
- Vigorous exercise 5+ hours/week CAN reduce fertility (by up to 32%)—but ONLY when combined with energy deficit
- Individual variation is huge—what works for one woman won't work for another
- Regular menstrual cycles are the best indicator that your exercise level is appropriate
- Exercise benefits fertility through multiple mechanisms beyond just weight management
When to Seek Help
See your GP or fertility specialist if:
- You've been trying for 12 months without success (under 35)
- You've been trying for 6 months without success (35+)
- Your periods are irregular or absent
- You're not ovulating regularly
- You have diagnosed PCOS, endometriosis, or other fertility issues
Don't wait if you have red flags—early intervention often involves simple adjustments to lifestyle (including exercise) rather than invasive treatments.
The Real Story
Here's the truth the internet won't tell you: Exercise is rarely the primary cause of infertility.
Age, male factor issues, PCOS, endometriosis, blocked tubes, ovulation disorders—these are far more common causes. For most women with regular periods and healthy BMI, exercise level isn't the limiting factor.
But exercise CAN be a piece of the puzzle for some women, particularly:
- Very lean athletes with energy deficits
- Women with PCOS who need more movement
- Women with obesity who benefit from increased activity
The key is knowing which category you fall into—and your menstrual cycle will tell you.
The Bottom Line
Don't stop exercising when TTC unless you have irregular periods, very low BMI, or signs of overtraining. Exercise supports fertility through hormone regulation, stress reduction, and metabolic health.
Don't exercise to exhaustion while undereating. If you're doing vigorous exercise 5+ hours per week, ensure adequate calorie intake. Your body needs energy reserves to support pregnancy.
Listen to your menstrual cycle. Regular periods (22-33 days) = your exercise level is probably appropriate. Irregular or absent periods = time to reassess.
Individual variation is massive. Don't compare yourself to others. What matters is YOUR body's response—not what worked for someone else.
Focus on overall health, not obsessive optimization. The mental health benefits of exercise often outweigh minor fertility concerns, especially if you have regular cycles.
And remember: as one fertility specialist wisely noted, "In light of the considerable mental and physical health benefits of regular exercise, we would advocate against indiscriminately discouraging highly active women from engaging in vigorous exercise while trying to conceive."
Disclaimer: This information is based on peer-reviewed studies and medical guidance, but isn't medical advice. If you have concerns about exercise and fertility, speak to your GP or fertility specialist.




