If you and your partner have been trying to conceive, you're not alone—and the issue may not be solely on one side. Here's something many couples don't realise: male factor infertility accounts for 40-50% of all infertility cases, with an additional 20-30% involving combined male and female factors. This means male reproductive health plays a crucial role in up to 70% of couples struggling to conceive.
The culprit in many cases? Oxidative stress—damage caused when reactive oxygen species overwhelm the body's natural antioxidant defences, harming sperm DNA, motility, and overall function. In fact, between 25% and 87% of male subfertility is attributed to this cellular damage.
But here's the encouraging news: A substantial body of scientific evidence suggests that targeted antioxidant supplementation may improve sperm parameters and pregnancy outcomes for couples attending fertility clinics. The most recent 2022 Cochrane systematic review analysed 90 randomised controlled trials involving 10,303 subfertile men, finding that antioxidant supplementation may be associated with improved live birth rates, clinical pregnancy rates, and sperm quality measures, though the certainty of this evidence remains low to very low.
This comprehensive guide examines the evidence for male fertility supplements available in the UK, exploring which interventions show the strongest scientific support, recommended dosages, potential mechanisms of action, and when medical evaluation is warranted.
Also see: Prenatal Vitamins UK: What You Actually Need When Trying to Conceive for female fertility and pregnancy nutrition.

Understanding Male Fertility and Oxidative Stress
How Sperm Quality Is Measured
Before we dive into supplements, it's important to understand what "good" sperm quality actually means. Male fertility assessment typically involves semen analysis, which evaluates several key parameters defined by the World Health Organization (WHO) 2021 reference values:
- Sperm concentration: ≥16 million per millilitre
- Total sperm count: ≥39 million per ejaculate
- Progressive motility: ≥30% of sperm moving forward
- Total motility: ≥40% of sperm showing any movement
- Morphology: ≥4% of sperm with normal shape
However, standard semen analysis may not reveal all fertility issues. Sperm DNA fragmentation—damage to the genetic material within sperm—can impair fertilisation and embryo development even when conventional parameters appear normal. Specialised testing can measure this DNA damage, which is often elevated in men experiencing oxidative stress.
The Role of Oxidative Stress
Reactive oxygen species (ROS) are molecules produced naturally during cellular metabolism. At physiological levels, ROS play essential roles in sperm capacitation and the acrosome reaction—processes required for successful fertilisation. However, when ROS production exceeds the buffering capacity of antioxidants, oxidative stress occurs.
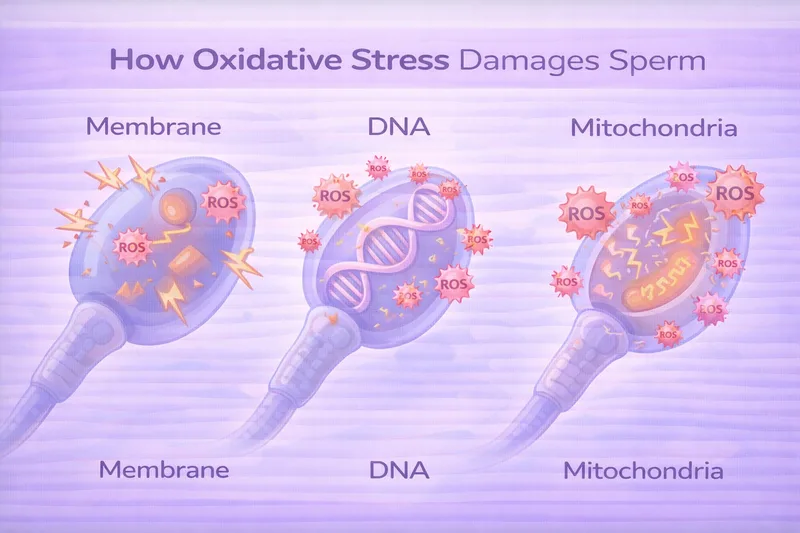
Oxidative stress damages sperm through multiple mechanisms:
- Lipid peroxidation of sperm membranes, reducing motility and viability
- Direct DNA damage through strand breaks and base modifications
- Impaired mitochondrial function, reducing energy production for sperm movement
- Protein oxidation affecting sperm structure and function
Common sources of elevated oxidative stress include:
- Infection and inflammation
- Varicocele (enlarged veins in the scrotum)
- Obesity
- Smoking
- Excessive alcohol consumption
- Environmental toxins
- Heat exposure
This explains why lifestyle factors can significantly impact male fertility—a topic we'll explore in detail later in this guide.
Evidence-Based Supplements for Male Fertility
Supplement Summary: Quick Reference
🥇 STRONGEST EVIDENCE:
CoQ10 (Coenzyme Q10)
→ Daily dose: 100–300 mg
→ Best for: Sperm concentration
→ Evidence: Strong (SUCRA ranking: 79.4%)
→ Key finding: Highest efficacy ranking for improving concentration
L-Carnitine
→ Daily dose: 500–1000 mg
→ Best for: Sperm motility
→ Evidence: Strong (SUCRA ranking: 88.7%)
→ Key finding: Most effective for motility (+12.43% vs placebo)
⭐ MODERATE TO STRONG EVIDENCE:
Selenium
→ Daily dose: 100–200 μg
→ Best for: Overall sperm quality
→ Evidence: Moderate-Strong
→ Key finding: Improved motility (+3.3%), concentration, morphology (+1.87%)
Zinc
→ Daily dose: 25–66 mg
→ Best for: Motility & concentration
→ Evidence: Moderate
→ Key finding: Increased motility (+7.03%), concentration (+1.48 M/mL)
→ Note: Large FAZST trial showed no benefit for zinc+folic acid combination
Vitamin C
→ Daily dose: 500–1000 mg
→ Best for: Sperm morphology
→ Evidence: Moderate
→ Key finding: Highest ranking for morphology (SUCRA: 93.6%)
Vitamin E
→ Daily dose: 400 IU
→ Best for: Pregnancy rates
→ Evidence: Moderate
→ Key finding: 8.17× increase in pregnancy rates (limited studies)
Omega-3 (EPA+DHA)
→ Daily dose: 1–2 g
→ Best for: Concentration & motility
→ Evidence: Moderate
→ Key finding: +10.98 M/mL concentration, +7.55% motility
NAC (N-Acetyl Cysteine)
→ Daily dose: 600 mg
→ Best for: DNA fragmentation
→ Evidence: Moderate
→ Key finding: Reduced DNA fragmentation in TUNEL assay
⚠️ MIXED EVIDENCE:
Folic Acid
→ Daily dose: 0.5–5 mg
→ Best for: Variable results
→ Evidence: Mixed
→ Note: Large FAZST trial showed no benefit as standalone supplement
💊 MULTI-ANTIOXIDANT FORMULATIONS:
Combined supplements
→ Evidence: Moderate-Strong
→ Example: Menevit study showed 38.5% vs 16% viable pregnancy rate in IVF
→ Typically contain: L-carnitine, CoQ10, vitamin C, vitamin E, selenium, zinc, folic acid
Important: Evidence levels reflect study quality and consistency, not guaranteed effectiveness. Individual responses to supplementation vary considerably, and not all men will experience the benefits observed in clinical trials.

Coenzyme Q10 (CoQ10)
Evidence Level: Strong for sperm parameters
Recommended Dosage: 100–300 mg daily
Coenzyme Q10 is a lipid-soluble antioxidant concentrated in mitochondria, where it plays crucial roles in cellular energy production and ROS neutralisation. Network meta-analysis comparing multiple antioxidants found CoQ10 achieved the highest efficacy ranking for improving sperm concentration in the studies analysed, with a SUCRA value of 79.4%, though individual responses may vary.
What the research shows:
Multiple randomised controlled trials demonstrate CoQ10's benefits. In one study of 60 infertile men with high DNA fragmentation, those receiving a multi-antioxidant formula containing CoQ10 showed significantly higher sperm density after 3 months compared to placebo (27.2 vs 24.4 million/mL).
Another trial found 200 mg daily CoQ10 for 3 months significantly increased:
- Sperm concentration from 8.22 to 12.53 million/mL (+52%)
- Progressive motility from 16.54% to 22.58% (+36%)
- Total motility from 25.68% to 29.96% (+17%)
A systematic review and meta-analysis published in Advances in Nutrition found CoQ10 supplementation significantly increased sperm concentration by 5.95 million/mL and sperm motility by 7.33% compared to placebo.
UK Availability: CoQ10 supplements are widely available in the UK from pharmacies (Boots, Superdrug), health food stores (Holland & Barrett), and online retailers. Look for ubiquinol (the reduced, active form) or ubiquinone. Most formulations contain 100–200 mg per capsule.
L-Carnitine and Acetyl-L-Carnitine
Evidence Level: Strong for sperm motility
Recommended Dosage: 500–1000 mg daily (L-carnitine), or combination with acetyl-L-carnitine
Carnitines facilitate fatty acid transport into mitochondria for energy production and possess antioxidant properties. Network meta-analysis identified carnitine as having the highest ranking for improving sperm motility among tested interventions (SUCRA: 88.7%), with studies showing a mean increase of 12.43% in motility compared to placebo, though results varied between studies.
What the research shows:
One prospective study of 20 infertile men with oligoasthenoteratozoospermia receiving 1500 mg L-carnitine daily for 3 months (combined with other antioxidants) demonstrated significant improvements in sperm concentration, motility, vitality, and morphology, alongside substantial reduction in DNA fragmentation.
Meta-analysis data show carnitine supplementation:
- Increases progressive motility by approximately 7.45%
- Improves sperm morphology by 4.91%
- Enhances total motility by 7.84%
UK Availability: L-carnitine and acetyl-L-carnitine supplements are readily available in the UK. Some formulations combine both forms. Typical capsules contain 250–500 mg.
Selenium
Evidence Level: Moderate to strong
Recommended Dosage: 100–200 μg daily
Selenium is an essential trace element required for spermatogenesis in mammals. It functions as a cofactor for glutathione peroxidase, a key antioxidant enzyme that protects sperm from oxidative damage. Selenium deficiency has been associated with impaired sperm motility and morphology.
What the research shows:
Meta-analysis of randomised controlled trials found selenium supplementation (100–300 μg daily for 3–11 months) significantly improved:
- Sperm total motility by 3.30%
- Sperm concentration by 3.91 million/mL
- Sperm morphology by 1.87%
A study comparing 200 mg CoQ10 versus 200 μg selenium daily for 3 months found both groups showed significant improvements in sperm parameters and antioxidant markers, though CoQ10 produced slightly greater effects.
UK Availability: Selenium supplements are available in the UK, typically as selenomethionine or sodium selenite. Most formulations provide 50–200 μg per tablet.
⚠️ Important: Do not exceed 400 μg daily from all sources, as excessive selenium can be toxic.
Zinc
Evidence Level: Moderate
Recommended Dosage: 25–66 mg daily (most studies use 25–66 mg)
Zinc plays pivotal roles in spermatogenesis, supporting Sertoli cell function and maintaining seminiferous epithelium structural integrity. It serves as a cofactor for enzymes involved in DNA synthesis, repair, and cellular division, while its antioxidant properties help counteract oxidative stress.
What the research shows:
Meta-analysis demonstrated that zinc supplementation (66–500 mg daily for 3–6 months) significantly:
- Increased sperm total motility by 7.03%
- Increased concentration by 1.48 million/mL
However, a large multicentre randomised controlled trial involving 2,370 infertile men found that 5 mg folic acid plus 30 mg zinc daily for 6 months did not improve sperm DNA fragmentation or live birth rates compared to placebo. This suggests zinc alone may not be sufficient, or that dosage and duration matter significantly.
UK Availability: Zinc supplements are widely available in the UK in various forms (zinc citrate, zinc picolinate, zinc gluconate). Typical formulations contain 15–50 mg.
⚠️ Important: Avoid exceeding 40 mg daily long-term without medical supervision, as excess zinc can interfere with copper absorption.
Vitamin C (Ascorbic Acid)
Evidence Level: Moderate for sperm morphology
Recommended Dosage: 500–1000 mg daily
Vitamin C is a water-soluble antioxidant found in high concentrations in seminal fluid, where it protects sperm from oxidative damage. Network meta-analysis suggested vitamin C may be most effective for improving sperm morphology (SUCRA: 93.6%), though the effect did not reach statistical significance compared to placebo in that particular analysis.
What the research shows:
Studies using vitamin C as part of combination antioxidant formulas have shown positive results. One trial found 90 mg vitamin C combined with vitamin E, CoQ10, selenium, and zinc for 3 months significantly enhanced sperm concentration and motility in men with idiopathic oligoasthenozoospermia.
UK Availability: Vitamin C is inexpensive and universally available in the UK. Most supplements provide 500–1000 mg per tablet. Higher doses may cause gastrointestinal discomfort in some individuals.
Vitamin E (Alpha-Tocopherol)
Evidence Level: Moderate
Recommended Dosage: 400 IU daily
Vitamin E is a lipid-soluble antioxidant that protects cell membranes from oxidative damage. It works synergistically with other antioxidants, particularly vitamin C and selenium. Meta-analysis found vitamin E supplementation associated with an 8.17-fold increase in pregnancy rates when used in fertility treatment, though this was based on limited studies.
What the research shows:
Randomised trials combining vitamin E with selenium, folic acid, or other antioxidants have shown improvements in sperm motility and functional parameters. One study of 60 men receiving selenium and vitamin E found significant improvements compared to placebo.
UK Availability: Vitamin E supplements are widely available in the UK as d-alpha-tocopherol (natural) or dl-alpha-tocopherol (synthetic). Most formulations contain 200–400 IU per capsule.
Folic Acid
Evidence Level: Mixed results
Recommended Dosage: 0.5–5 mg daily
Folic acid is essential for DNA synthesis and methylation processes. Some meta-analyses have reported a 3.38-fold increase in pregnancy rates with folic acid supplementation.
However, the large FAZST trial involving 2,370 men found 5 mg folic acid plus 30 mg zinc daily did not improve sperm DNA fragmentation or fertility outcomes compared to placebo, casting doubt on folic acid's efficacy as a standalone intervention for male fertility.
Folic acid may be more beneficial when combined with other antioxidants or in men with folate deficiency.
UK Availability: Folic acid is inexpensive and widely available. Standard supplements contain 400 μg, though higher-dose formulations (5 mg) are also available.
Omega-3 Fatty Acids
Evidence Level: Moderate
Recommended Dosage: 1–2 g EPA+DHA daily
Omega-3 polyunsaturated fatty acids (particularly EPA and DHA) are incorporated into sperm membranes, influencing fluidity and function.
What the research shows:
Meta-analysis found omega-3 supplementation significantly:
- Increased total sperm concentration by 10.98 million/mL
- Increased total sperm count by 18.70 million
- Increased total motility by 7.55%
- Improved morphology by 0.91%
UK Availability: Fish oil and algae-based omega-3 supplements are widely available. Look for products standardised to EPA and DHA content rather than total fish oil weight.
N-Acetyl Cysteine (NAC)
Evidence Level: Moderate
Recommended Dosage: 600 mg daily
NAC is a precursor to glutathione, the body's master antioxidant. It has been shown to reduce sperm DNA fragmentation measured by TUNEL assay after 3 months of treatment. Pairwise meta-analysis found NAC showed statistically significant improvements compared to placebo.
UK Availability: NAC supplements are available in the UK from health food stores and online. Typical formulations contain 600 mg per capsule.
Multi-Antioxidant Formulations
Evidence Level: Moderate to strong
Many clinical trials have used combination antioxidant formulations rather than single agents. The rationale is that oxidative stress is a multifaceted problem that may benefit from targeting multiple pathways simultaneously.
What the research shows:
Commercial fertility supplements such as Menevit contain validated combinations. One study found Menevit improved viable pregnancy rates from 16% to 38.5% in couples undergoing IVF-ICSI where male partners had evidence of oxidative stress.
Examples from research include combinations of:
- L-carnitine
- CoQ10
- Vitamin C
- Vitamin E
- Selenium
- Zinc
- Folic acid
UK Availability: Several male fertility supplements are available in the UK containing antioxidant combinations. Check labels to ensure they contain therapeutic doses of key ingredients like CoQ10 (≥100 mg), L-carnitine (≥500 mg), selenium (≥100 μg), and zinc (≥25 mg).

Lifestyle Factors Affecting Male Fertility
While supplements may offer some benefit, addressing modifiable lifestyle factors is equally—if not more—important for male fertility. Environmental, occupational, and behavioural factors can significantly impact sperm quality through oxidative stress, hormonal disruption, and direct cellular damage.
Smoking 🚬
Impact: Severe
Cigarette smoking has well-established detrimental effects on male fertility. Meta-analysis of 57 studies involving 29,914 participants found smoking associated with:
- Decreased semen volume (−0.25 mL)
- Decreased total sperm count (−32.2 million/mL)
- Decreased concentration (−7.1 million/mL)
- Decreased normal morphology (−1.9%)
- Decreased motility (−4.9%)
Smoking increases sperm DNA fragmentation, impairs spermatogenesis through hypoxia, and increases testosterone metabolism in the liver, causing secretory dysfunction of Leydig and Sertoli cells.
✅ Recommendation: Complete smoking cessation. Evidence suggests quitting smoking can improve sperm parameters, though the timeline for recovery varies.
Alcohol Consumption 🍺
Impact: Moderate to severe (dose-dependent)
Excessive alcohol intake adversely affects testosterone metabolism, spermatogenesis, and increases DNA damage in male germ cells. Studies show heavy alcohol users have substantially higher leukocyte concentrations in seminal fluid and altered free oestradiol to free testosterone ratios.
One study found only 12% of alcoholics showed normal semen parameters compared to 37% of non-alcoholic, non-smoker controls. Teratozoospermia (abnormal morphology) and oligozoospermia (low count) were particularly common in regular drinkers.
✅ Recommendation: Limit alcohol consumption. While moderate intake may not significantly harm fertility, heavy drinking (>14 units per week) should be avoided when trying to conceive.
Obesity and Weight 📊
Impact: Moderate to severe
Elevated body mass index is associated with decreased sperm concentration, motility, and increased DNA damage, though the relationship is complex. Obesity is linked to metabolic syndrome, which may reduce testosterone levels and increase oestradiol through aromatase activity in adipose tissue. Excess adiposity may also elevate scrotal temperature and promote chronic inflammation, potentially exacerbating oxidative stress.
Studies suggest men with higher BMI are more likely to have reduced fertility parameters compared to those within the healthy weight range. Weight reduction through dietary changes and regular physical activity may improve semen quality and hormonal balance in some men.
✅ Recommendation: Achieve and maintain a healthy BMI (18.5–24.9 kg/m²). Even modest weight loss in obese men can improve fertility parameters.
Heat Exposure 🔥
Impact: Moderate
Elevated scrotal temperature impairs spermatogenesis. The testes function optimally at temperatures slightly below core body temperature (approximately 2–4°C cooler). Prolonged heat exposure from hot tubs, saunas, tight clothing, laptop use on the lap, or occupational environments can reduce sperm production and motility.
✅ Recommendation:
- Avoid prolonged exposure to heat sources
- Limit hot bath and sauna use
- Avoid placing laptops directly on the lap for extended periods
- Wear loose-fitting underwear
- Take regular breaks if working in hot environments
Psychological Stress 😰
Impact: Moderate
Chronic stress may affect male fertility through hormonal disruption and oxidative stress pathways. Stress can potentially lower testosterone levels and impair sexual function. Studies suggest psychological stress may correlate with reduced sperm motility, viability, and concentration, though the relationships are complex and multifactorial.
✅ Recommendation: Implement stress-reduction techniques such as regular exercise, adequate sleep (7–9 hours), mindfulness practices, and professional counselling if needed. The fertility journey itself can be stressful; couples should seek support when appropriate.
Physical Activity 🏃
Impact: Positive (moderate activity)
Regular moderate physical activity has been associated with better sperm motility and overall sperm quality in some studies. Exercise may help maintain healthy weight, reduce oxidative stress, and support hormonal balance. However, the relationship is complex, and excessive intense exercise may have negative effects in some individuals, particularly when combined with other risk factors.
✅ Recommendation: Engage in regular moderate exercise (150 minutes per week of moderate-intensity activity). Avoid excessive endurance training or anabolic steroid use.
Diet and Nutrition 🥗
Impact: Moderate to strong
A diet rich in fruits, vegetables, whole grains, seeds, nuts, and fish may support sperm health through natural antioxidants and omega-3 fatty acids. The Mediterranean diet pattern has been associated with better male fertility in observational studies and may offer some protection against environmental pollutant-induced fertility decline, though more research is needed to establish causation.
Conversely, high consumption of sugar, processed foods, red meat, and soy products has been associated with poorer fertility outcomes in some studies, though evidence is mixed.
✅ Recommendation: Follow a balanced diet emphasising:
- Plenty of vegetables and fruits (antioxidant-rich)
- Whole grains
- Lean proteins, particularly fish (omega-3 source)
- Nuts and seeds
- Healthy fats (olive oil, avocado)
Limited processed foods, sugar, and red meat

When to Seek Medical Evaluation
While lifestyle modifications and supplements may help, certain circumstances warrant professional medical assessment:
When to See Your GP
You should seek medical evaluation if:
- ❌ Inability to conceive after 12 months of regular unprotected intercourse (or 6 months if female partner is over 35)
- ❌ Known risk factors: history of undescended testes, previous testicular surgery or injury, varicocele, sexually transmitted infections, or childhood mumps
- ❌ Sexual dysfunction: erectile difficulties, premature ejaculation, or pain during intercourse
- ❌ Abnormal physical findings: testicular lumps, swelling, or pain
- ❌ Hormonal symptoms: low libido, reduced facial/body hair, breast enlargement (gynaecomastia)
Your GP can arrange initial investigations including semen analysis and hormone testing (testosterone, FSH, LH). Depending on results, referral to a urologist or fertility specialist may be appropriate.
NHS Fertility Services
In the UK, NHS fertility services are available, though eligibility criteria vary significantly by Integrated Care Board (ICB). NICE guidelines recommend 3 IVF cycles for eligible women under 40, but in practice nearly 70% of ICBs now only fund 1 cycle, creating a "postcode lottery":
- Women under 40: Typically 1 cycle (though NICE recommends 3; only 2 ICBs in England follow this guidance)
- Women aged 40-42: Typically 1 cycle
- Criteria often include: not smoking, healthy BMI (19–30), no existing children from either partner
Private fertility treatment is also available throughout the UK if you don't meet NHS criteria or prefer quicker access.
Semen Analysis
Standard semen analysis evaluates volume, concentration, motility, and morphology according to WHO 2021 criteria. Two separate samples collected 2–4 weeks apart are typically recommended, as sperm parameters can vary significantly between ejaculates.
If standard analysis is normal but fertility issues persist, specialised tests may be considered:
- Sperm DNA fragmentation testing (TUNEL, SCSA, SCD)
- Anti-sperm antibody testing
- Oxidative stress measurement
- Genetic testing (if indicated: karyotype, Y-chromosome microdeletions, cystic fibrosis screening)
Treatment Options
Medical interventions for male infertility depend on the underlying cause and may include:
- Lifestyle modification (first-line for many men)
- Antioxidant supplementation (as discussed in this guide)
- Hormonal therapy (for hypogonadism or other hormonal imbalances)
- Surgical intervention (varicocele repair, vasectomy reversal, treatment of obstructions)
- Assisted reproductive technology (IUI, IVF, ICSI)
Interpreting the Evidence: What the Research Really Shows
The 2022 Cochrane systematic review—the gold standard in evidence synthesis—provides the most comprehensive assessment of antioxidant supplementation for male subfertility. Based on 90 randomised controlled trials with 10,303 men, the review concluded:
Key Findings
📊 Very low-certainty evidence suggests antioxidant supplementation may be associated with improved live birth rates for subfertile couples attending fertility clinics.
What this means in numbers:
- Without antioxidants: 16 out of 100 couples achieve live birth
- With antioxidants: Between 17 and 27 out of 100 couples may achieve live birth
📊 Low-certainty evidence suggests clinical pregnancy rates may increase with antioxidant use.
📊 There is no evidence of increased miscarriage risk, though antioxidants may cause mild gastrointestinal discomfort based on very low-certainty evidence.
⚠️ Importantly, when studies with high risk of bias were removed from analysis, the evidence for increased live births disappeared, highlighting significant methodological concerns in the existing research base.
Why "Low Certainty" Evidence?
The certainty of evidence is downgraded due to:
- ❌ Serious risk of bias from poor reporting of randomisation methods
- ❌ Failure to report key clinical outcomes (live birth, clinical pregnancy)
- ❌ High attrition rates (participant drop-out) in some studies
- ❌ Imprecision due to low event rates and small sample sizes
- ❌ Heterogeneity in study populations, interventions, and outcome measures
This doesn't mean antioxidants don't work—it means we can't be highly confident in the precise magnitude of benefit. More rigorous studies are needed.
Current Guidelines
European Association of Urology (EAU) and American Urological Association (AUA) guidelines acknowledge that while antioxidants may improve sperm parameters and appear to be generally safe, conclusive data demonstrating improved fertility outcomes remain lacking.
Most guidelines suggest antioxidants can be considered as part of a comprehensive approach, but emphasise they should not replace thorough fertility evaluation or evidence-based medical treatments. The guidelines generally recommend discussing potential benefits and limitations with patients on an individual basis.
Practical Recommendations for Men Trying to Conceive
Based on current evidence, men attempting to conceive may wish to consider the following steps to potentially optimise fertility. It is important to note that individual responses vary, and these recommendations should be discussed with a healthcare provider:
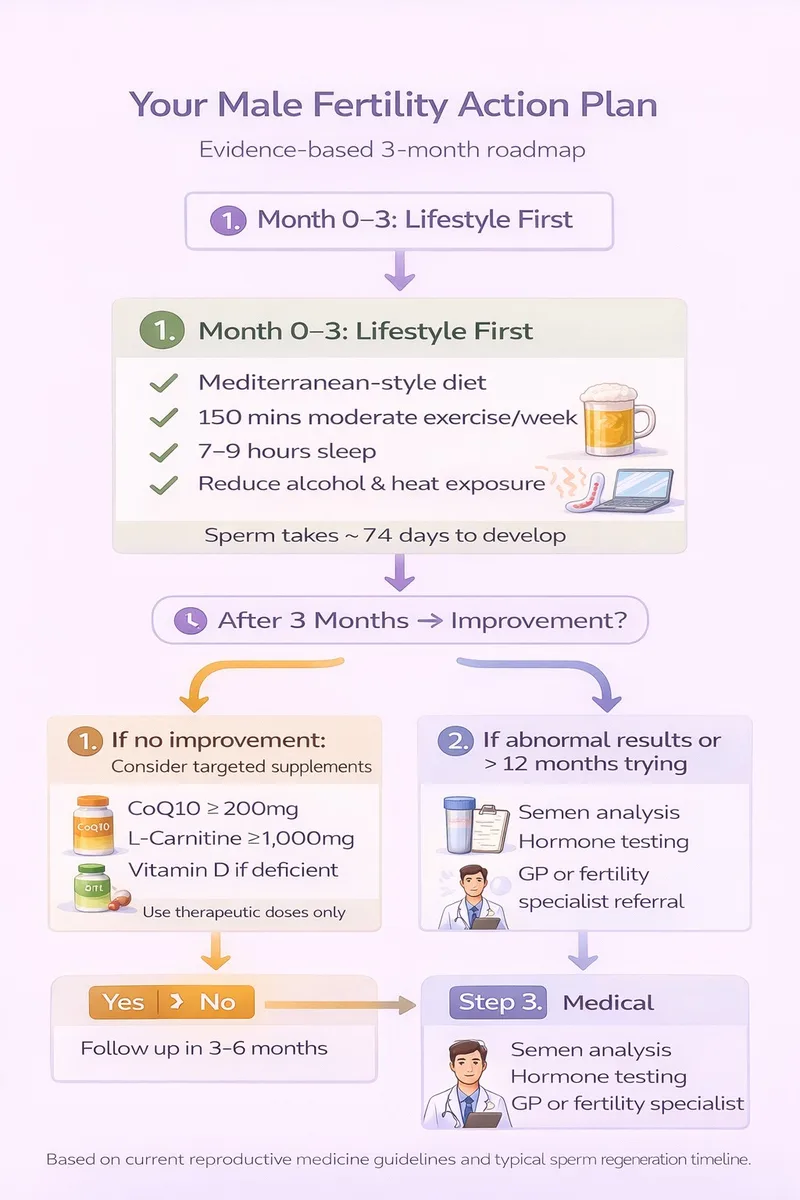
Priority 1: Lifestyle Modification ⭐⭐⭐
These changes have the strongest evidence and should be implemented first:
- ✅ Stop smoking immediately (strongest negative impact)
- ✅ Reduce alcohol to ≤14 units per week or less
- ✅ Achieve healthy weight (BMI 18.5–24.9)
- ✅ Avoid heat exposure (hot tubs, saunas, tight underwear, laptops on lap)
- ✅ Regular moderate exercise (150 minutes per week)
- ✅ Mediterranean-style diet (fruits, vegetables, fish, nuts, whole grains)
- ✅ Manage stress (sleep 7–9 hours, relaxation techniques, support)
Priority 2: Consider Antioxidant Supplementation ⭐⭐
If lifestyle factors are optimised and you wish to try supplements, understanding that individual responses vary:
Option 1: Multi-Antioxidant Formulation (Most Evidence)
Look for products containing therapeutic doses of:
- CoQ10: 100–200 mg
- L-carnitine: 500–1000 mg
- Selenium: 100–200 μg
- Zinc: 25–50 mg
- Vitamin C: 500–1000 mg
- Vitamin E: 400 IU
UK Examples: Conception Men, Proceive Men, Vitabiotics Wellman Conception
Option 2: Individual Supplements
If you prefer targeted supplementation:
To improve sperm concentration:
→ Take: CoQ10
→ Dosage: 200 mg daily
To improve sperm motility:
→ Take: L-carnitine
→ Dosage: 500–1000 mg daily
To support overall quality:
→ Take: Selenium
→ Dosage: 200 μg daily
To support multiple parameters:
→ Take: Omega-3 (fish oil)
→ Dosage: 1–2 g EPA+DHA daily
Important Supplement Considerations
⏱️ Timeline: Spermatogenesis takes approximately 74 days; allow at least 3 months before expecting improvements
📅 Duration: Most research trials used supplements for 3–6 months
💊 Safety: Check with your GP if you have medical conditions or take medications, as some supplements can interact
🏷️ Quality: Supplements are not regulated like medications; choose reputable brands with third-party testing
⚠️ Effectiveness: Not all men respond to supplementation. The evidence shows average improvements across groups, but individual results vary considerably. Some men may experience significant benefits, while others may see little to no change.
Priority 3: Seek Medical Evaluation ⭐
If pregnancy doesn't occur after:
- 12 months of trying (or 6 months if partner is over 35)
- Both partners should undergo fertility evaluation
Male assessment includes:
- Semen analysis (two samples, 2–4 weeks apart)
- Hormonal testing (testosterone, FSH, LH)
- Physical examination
- Specialised tests if needed (DNA fragmentation, genetic testing)
Early investigation allows for timely intervention.
Frequently Asked Questions
How long does it take for supplements to improve sperm quality?
Sperm production (spermatogenesis) takes approximately 74 days (about 2.5 months). Most clinical trials showing positive results used supplements for 3–6 months. You should allow at least 3 months of consistent supplementation before assessing effectiveness through repeat semen analysis. However, it's important to note that individual responses vary considerably, and not all men will experience measurable improvements.
Can I take multiple supplements together?
Yes, many studies showing positive results used combination formulations containing multiple antioxidants. In fact, multi-antioxidant formulations often show stronger evidence than single supplements. However:
- Avoid exceeding maximum safe doses (e.g., selenium >400 μg/day, zinc >40 mg/day long-term)
- Be cautious of duplicate ingredients if taking multiple products
- Consult your GP if you take medications or have health conditions
Do I need a semen analysis before taking supplements?
Not required, but highly recommended if:
- You've been trying to conceive for over 6–12 months
- You want to measure the effectiveness of lifestyle changes or supplements
- You have known risk factors for male infertility
A baseline semen analysis allows you to track improvements objectively.
Will my partner's prenatal vitamins affect my fertility?
No, your partner's prenatal vitamins (e.g., folic acid, vitamin D) are designed for female reproductive health and pregnancy. You need male-specific supplements targeting sperm quality and oxidative stress.
See also: Prenatal Vitamins UK: What You Actually Need When Trying to Conceive for female fertility nutrition.
Are expensive fertility supplements better than basic vitamins?
Not necessarily. What matters is:
- Therapeutic dosages of active ingredients (check the label!)
- Quality and purity (third-party testing, reputable manufacturer)
- Evidence-based ingredients (CoQ10, carnitine, selenium, zinc, etc.)
Some expensive products contain effective doses; some don't. Similarly, some budget options are good value; others are underdosed. Always check the label against the dosages mentioned in this guide.
Can supplements replace a healthy lifestyle?
No. Supplements are supplementary—they may work best when combined with:
- Smoking cessation
- Alcohol moderation
- Healthy weight
- Regular exercise
- Nutritious diet
- Stress management
Lifestyle factors have stronger and more consistent evidence and provide broader health benefits. Supplements should be viewed as a potential complement to, not a replacement for, healthy lifestyle habits.
Do I need to stop supplements once my partner is pregnant?
Yes, you can stop. Once pregnancy is confirmed:
- Sperm quality no longer affects the pregnancy outcome
- Focus shifts to supporting your partner
- You can discontinue fertility supplements
However, maintaining healthy lifestyle habits benefits your overall health and any future conception attempts.
What if my semen analysis is normal but we still can't conceive?
Standard semen analysis doesn't measure everything. Consider:
- Sperm DNA fragmentation testing (not included in standard analysis)
- Female partner evaluation (ovulation, fallopian tubes, uterine health)
- Timing and frequency of intercourse during fertile window
- Specialist consultation if trying >12 months
Remember: male AND female factors need assessment.
Are there any side effects from male fertility supplements?
Most antioxidants are well-tolerated. Possible mild side effects include:
- Gastrointestinal discomfort (CoQ10, NAC, high-dose vitamin C)
- Fishy aftertaste (omega-3, if not high quality)
- Nausea (zinc on empty stomach)
Serious side effects are rare at recommended doses. Stop and consult your GP if you experience:
- Persistent digestive issues
- Allergic reactions
- Unusual symptoms
Can I get these nutrients from food alone?
Partially, but difficult to reach therapeutic levels shown in research:
CoQ10 (200 mg):
→ Food equivalent: ~3 kg beef heart daily
L-carnitine (1000 mg):
→ Food equivalent: ~500g red meat daily
Selenium (200 μg):
→ Food equivalent: ~3–4 Brazil nuts daily*
→ *Note: Brazil nut selenium content varies widely by soil
Omega-3 (2 g EPA+DHA):
→ Food equivalent: ~100g fatty fish 3× per week
A nutrient-rich diet provides a foundation, but supplements achieve the specific therapeutic levels tested in fertility research.
Conclusion
Male fertility is influenced by a complex interplay of genetic, hormonal, environmental, and lifestyle factors. While oxidative stress appears to play a significant role in many cases of male subfertility, the evidence for antioxidant supplementation, though generally positive in direction, remains of low to moderate certainty.
All scientific evidence cited in this article is hyperlinked throughout the text. Click any linked study to access the full research on PubMed.
Current evidence suggests potential benefits from:
✅ CoQ10 for improving sperm concentration (100–300 mg daily)
✅ L-Carnitine for motility (500–1000 mg daily)
✅ Multi-antioxidant combinations for overall sperm parameters
✅ Lifestyle modification as the foundation (smoking cessation, alcohol moderation, healthy weight, exercise, Mediterranean diet)
However, lifestyle modification—particularly smoking cessation, alcohol moderation, weight management, and dietary improvement—appears to have the strongest evidence base and should be considered the foundation of any fertility enhancement strategy. These changes have broader health benefits extending well beyond fertility.
Your Action Plan
Consider starting with:
- Eliminate harmful habits (smoking, excessive alcohol)
- Optimise your health (weight, exercise, diet, sleep)
- Consider evidence-based supplements (after 1–3 months of lifestyle changes, if appropriate)
- Seek medical evaluation if pregnancy hasn't occurred after 12 months of trying
Remember: Fertility is a shared journey. Both partners' health matters, and improving male fertility parameters through evidence-based interventions may increase the likelihood of successful conception, though outcomes vary between individuals.
If you and your partner have been trying to conceive for over 12 months (or 6 months if she's over 35), don't delay seeking professional help. Early evaluation and intervention provide the best outcomes.
Related Articles:
- Prenatal Vitamins UK: What You Actually Need When Trying to Conceive
- When to See a Fertility Doctor UK: Guide for Trying to Conceive
- Understanding Semen Analysis Results: A Complete UK Guide
Medical Disclaimer This article is for informational and educational purposes only and is not intended as medical advice. Male infertility can have various underlying causes that require professional diagnosis and treatment. Always consult with your GP or a qualified fertility specialist before starting any supplement regimen, especially if you have existing medical conditions, take medications, or have been trying to conceive for over 12 months. The information provided should not replace professional medical consultation or delay seeking appropriate care.