The 20 week scan is one of those pregnancy milestones that sits in a strange space between excitement and anxiety. You want to see your baby. You want to know everything is okay. But somewhere in the back of your mind, there's a quiet fear about what might be found.
I remember sitting in the waiting room with my partner, trying to act calm while silently bricking it. I had read every forum thread about anomaly scans and was convinced the sonographer's silence would mean something terrible. In the end, the scan was fine — but nobody had told us what to actually expect, and that made the whole thing more stressful than it needed to be.
This guide is what we wish someone had given us beforehand. We'll cover what the scan checks for, what actually happens in the room, what the sonographer is looking at, and what happens if something unexpected is found.
What Is the 20 Week Scan?
The 20 week scan — officially called the fetal anomaly scan or mid-pregnancy scan — is a detailed ultrasound offered to all pregnant women on the NHS as part of routine antenatal care. It is usually done between 18 and 21 weeks of pregnancy. The recommended NHS screening window is 18+0 to 20+6 weeks.
According to NICE guideline NG201, pregnant women should be offered an ultrasound scan between 18+0 and 20+6 weeks to screen for fetal anomalies as part of the NHS Fetal Anomaly Screening Programme (FASP).
This is not just a chance to see your baby — although that's a wonderful part of it. The primary purpose of the scan is to check your baby's physical development in detail and to screen for a number of specific conditions. It also checks the position of the placenta, the fluid around your baby, and your baby's size at that stage.
It's important to understand that this is a screening test, not a diagnostic one. That means it can identify signs that may suggest a condition, but it cannot detect everything, and in most cases the scan will show that your baby appears to be developing normally.
What Does the Scan Check For?

The NHS FASP screens for 11 specific physical conditions during the anomaly scan. Detection rates vary depending on the condition, and the scan cannot guarantee that all abnormalities will be found. The conditions screened for include:
Anencephaly, a condition affecting brain development. Open spina bifida, where the spine does not close properly — the NHS notes that this can typically be detected in around 9 out of 10 cases. Cleft lip, a gap in the upper lip that may extend to the palate. Diaphragmatic hernia, where a hole in the diaphragm affects lung development. Gastroschisis, where the intestines develop outside the abdomen. Exomphalos, where abdominal organs protrude through the area where the umbilical cord meets the belly. Serious cardiac abnormalities — the Gov.uk screening programme guidance acknowledges that heart conditions are more difficult to detect, with approximately half (around 50%) identified at the scan. Bilateral renal agenesis, the absence of both kidneys. Lethal skeletal dysplasia, a severe condition affecting bone development. Edwards' syndrome (Trisomy 18) and Patau's syndrome (Trisomy 13), two rare chromosomal conditions.
The Gov.uk FASP guidance notes that detection rates vary significantly depending on the type of condition. Some — such as gastroschisis and anencephaly — tend to be detected at very high rates, while others — including certain cardiac malformations — remain more challenging to identify through ultrasound screening.
It's worth remembering that these conditions are rare. In the large majority of scans, the sonographer will confirm that your baby appears to be developing as expected.
What Actually Happens on the Day
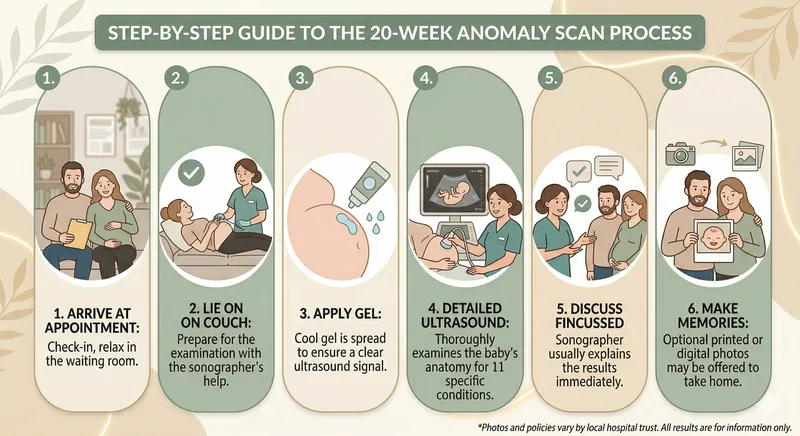
Knowing what to expect can take some of the anxiety away. Here's what typically happens.
Before the scan: Your midwife will have booked the appointment for you, usually at your local hospital or maternity unit. Some hospitals may ask you to arrive with a full bladder, as this can help provide a clearer image of the baby — check with your unit beforehand. Wear comfortable clothing that allows easy access to your abdomen. You can bring your partner or a support person, but most hospitals do not allow children in the scan room.
In the scan room: The room will be dimly lit to help the sonographer see the ultrasound images clearly. You'll be asked to lie on a couch and lift or lower your clothing so your abdomen is exposed. Tissue paper will be tucked into your waistband to protect your clothes, and a cool gel will be applied to your belly.
During the scan: The sonographer will move a handheld device called a transducer across your abdomen. They will be examining your baby's anatomy in detail — brain, spine, face, heart, kidneys, limbs, and abdomen — as well as checking your placenta position and amniotic fluid levels. According to the NHS, the scan usually takes around 30 minutes, though it may take longer if your baby is in an awkward position.
The silence: This is the part nobody warns you about. The sonographer will likely be quiet for extended periods while they concentrate on getting the images they need. This does not mean something is wrong — they are simply focused on a detailed and methodical examination. Sometimes another member of staff may be asked to review the images. This can happen for routine reasons and does not necessarily mean something is wrong.
After the scan: In most cases, the sonographer will tell you the results at the time of the scan. If everything appears normal, they will let you know. You may be offered photos of your baby — some hospitals charge a small fee for printed images.
What If Something Is Found?
If the sonographer identifies something unexpected, or if they are unable to get clear images of a particular area, they will explain what they have seen and what happens next. This might involve a second opinion from another member of staff, a follow-up scan at a later date, or referral to a fetal medicine specialist for more detailed imaging.
According to the Gov.uk FASP guidance, if one of the 11 screened conditions is suspected or identified, providers must make timely referrals to a local or tertiary-level centre as clinically appropriate. The screening pathway must be completed by 23+0 weeks.
It's important to know that being referred for further investigation does not necessarily mean there is a serious problem. Sometimes the baby's position makes it difficult to see certain structures clearly, or a follow-up scan is needed simply to confirm that an initial observation is nothing to worry about.
If difficult news is received, support is available. Antenatal Results and Choices (ARC) is a UK charity that offers non-directive support and information for parents who receive unexpected results from prenatal screening. Your maternity team can also connect you with specialist midwives and counselling services.
Can You Find Out the Sex of Your Baby?
In many cases, the sex of your baby can be identified during the anomaly scan. However, this is not the primary purpose of the scan, and the NHS FASP does not require fetal sex to be determined.
Whether or not you are told depends on your hospital's policy — some NHS trusts will tell you if you ask, while others will not. The baby's position can also make it impossible to see clearly, and the sonographer may not be able to confirm either way. If finding out the sex is important to you, check with your hospital in advance and understand that it cannot always be guaranteed.
What If the Scan Is Incomplete?
Sometimes the sonographer cannot get all the images they need. This may be because your baby is in an awkward position, is moving a lot, or because factors such as body mass index or the position of the placenta make certain views difficult to obtain. According to the NHS, this does not mean there is anything wrong — you may simply be asked to go for a short walk or have a drink and come back, or you may be offered a second appointment before 23 weeks.
If all the views cannot be obtained, you should usually be offered one repeat scan, and the screening pathway should be completed by 23+0 weeks.
What the Scan Cannot Tell You
It's important to have realistic expectations about what the anomaly scan can and cannot detect. While it is a detailed and valuable screening tool, it has limitations.
The scan cannot detect all possible conditions. Some abnormalities may not be visible at 20 weeks, or may only become apparent later in pregnancy or after birth. The Gov.uk screening guidance notes that detection rates vary by condition — some conditions are identified in the vast majority of cases, while others, particularly certain heart defects, are detected in roughly half of affected pregnancies.
The scan does not assess brain function, intellectual development, or how your baby will develop after birth. It is a structural check — it looks at how the body and organs have formed, not how they will function.
A normal scan result is reassuring, but it does not guarantee a completely healthy baby. There is always a small possibility that a condition may be present that could not be seen on ultrasound.
How to Prepare
There are a few practical things you can do to prepare:
Check with your hospital whether you need a full bladder for the appointment. Wear loose, comfortable clothing — a two-piece outfit makes it easier to access your belly. Bring your maternity notes with you. If your partner or support person is coming, confirm with the hospital how many people can attend. Think about whether you want to know the sex of your baby and discuss this with your partner beforehand. Consider whether you'd like printed photos — and bring change or a card in case there is a fee.
If you tend to feel anxious, it may help to remember that this is a routine part of antenatal care, and sonographers perform these scans every day.
The Bottom Line
The 20 week anomaly scan is one of the most important appointments in your pregnancy. It provides a detailed look at how your baby is developing and screens for a number of specific conditions — most of which are rare.
In most cases, the scan will show that your baby appears to be developing as expected. If something unexpected is found, you will be supported through the next steps by your maternity team and, if needed, specialist services.
It's normal to feel nervous beforehand. It's normal for the room to feel quiet. And it's completely normal to cry with relief — or just emotion — when you see your baby on the screen.
Go in knowing what to expect, and the experience will feel a lot less daunting than the internet might have led you to believe.
This article is for general information only and does not replace advice from your midwife, GP, or healthcare provider. If you have any concerns about your pregnancy or your baby's development, always contact your maternity team.
This article was written in April 2026. We regularly review our content against the latest NHS and NICE guidelines to help ensure accuracy. This article references NHS: 20-week Screening Scan (last reviewed 2 February 2023), NICE guideline NG201: Antenatal Care (published August 2021, last reviewed December 2024), Gov.uk: NHS Fetal Anomaly Screening Programme — 20-week Screening Scan (updated January 2026), and Antenatal Results and Choices (ARC). For further reading on detection rates across UK NHS trusts, see this population-based study of over one million pregnancies in PLOS Medicine (2025). If you have any concerns about your pregnancy or your baby's development, please speak to your midwife, GP, or maternity unit.



