Nobody tells you that one day you might struggle to walk to the bathroom. Or that turning over in bed will make you gasp. Or that putting your socks on will feel like an extreme sport.
Pelvic girdle pain — often still called SPD — is one of the most common and most underestimated conditions in pregnancy. It can range from a mild niggle to pain so severe that it affects everything you do. And too many women are told to "just get on with it" when there is actually treatment available that can help.
I started limping at about 30 weeks and assumed it was normal pregnancy aches. By 34 weeks I could barely get up the stairs. Nobody had mentioned PGP to me until I brought it up myself — and when I did, the physiotherapy referral made a real difference.
Quick answer: Pelvic girdle pain (PGP) affects up to 1 in 5 pregnant women. It is caused by the pelvic joints moving unevenly or becoming less stable. According to the RCOG, early diagnosis and treatment can relieve pain, and treatment is safe at any stage during or after pregnancy.
What Is Pelvic Girdle Pain?
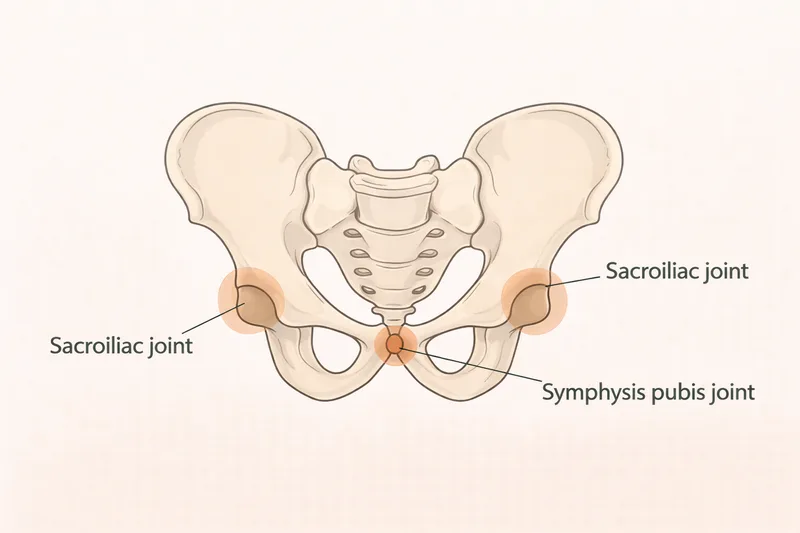
Your pelvis is a ring of bones at the base of your spine, held together by three joints — two sacroiliac joints at the back and the symphysis pubis joint at the front. These joints normally move very slightly and work together.
During pregnancy, changes in the body can affect how the pelvic joints move. In some women, the joints start moving unevenly, which can make the pelvic girdle less stable and painful. — your body's way of preparing for birth. In most women, this happens without problems. But in some, the joints start moving unevenly, which can make the pelvic girdle less stable and painful.
According to the NHS, PGP is a collection of uncomfortable symptoms caused by stiffness of the pelvic joints or the joints moving unevenly. The condition used to be called symphysis pubis dysfunction (SPD), and you may still hear that term used.
The RCOG notes that PGP is common, affecting around 1 in 5 pregnant women, and can affect mobility and quality of life. It can develop at any stage of pregnancy, though it is more common later on.
What Does PGP Feel Like?
PGP varies from person to person. For some women it is a mild ache; for others it can be severe enough to need crutches or a wheelchair. According to the RCOG, common symptoms include pain in the pubic region, lower back, hips, groin, thighs, or knees. Some women also feel or hear a clicking or grinding sensation in the pelvic area.
The pain tends to be worst during specific movements rather than constant. Activities that commonly aggravate PGP include walking — especially on uneven ground or for long distances, climbing stairs, turning over in bed, getting in and out of the car, standing on one leg — for example when getting dressed, and opening your legs wide.
According to the NHS, PGP is not harmful to your baby, but it can be painful and make it hard to get around. That last point matters — because too many women are told "it's just pregnancy" when there is help available.
What Causes It?
The exact cause is not fully understood. According to Tommy's, doctors and researchers do not understand exactly why PGP happens. But several factors are thought to contribute.
Hormonal changes. Pregnancy hormones — particularly relaxin — soften the ligaments around the pelvic joints. This is a normal part of pregnancy, but in some women the resulting joint laxity leads to instability and pain.
Uneven joint movement. The RCOG explains that PGP is usually caused by the pelvic joints moving unevenly, which makes the pelvic girdle less stable.
The weight and position of the baby. As your baby grows, the extra weight and the change in the way you sit, stand, and move puts more strain on the pelvis.
Previous injury or hypermobility. The RCOG notes that you are more likely to develop PGP if you have had a back problem or pelvic injury in the past, or if you have hypermobility syndrome — a condition in which your joints stretch more than normal.
Getting Diagnosed
If you are experiencing pelvic pain, tell your midwife or GP. The NHS advises that getting diagnosed as early as possible can help keep pain to a minimum and avoid long-term discomfort.
Your midwife or GP can refer you to a physiotherapist who specialises in obstetric pelvic problems. The RCOG states that this assessment will involve looking at your posture and your back and hip movements, and ruling out other causes of pelvic pain.
Do not wait for the pain to become severe before asking for help. PGP is treatable at any stage of pregnancy, and the sooner you are referred, the sooner you can start managing it.
What Can Help?
Treatment depends on the severity of your symptoms. According to the RCOG, your physiotherapist may suggest advice on avoiding movements that aggravate pain, exercises to strengthen your pelvic floor and abdominal muscles, manual therapy — hands-on treatment to the muscles and joints by a physiotherapist, osteopath, or chiropractor who specialises in PGP in pregnancy, and a pelvic support belt in some cases.
There are also practical things you can do day to day:
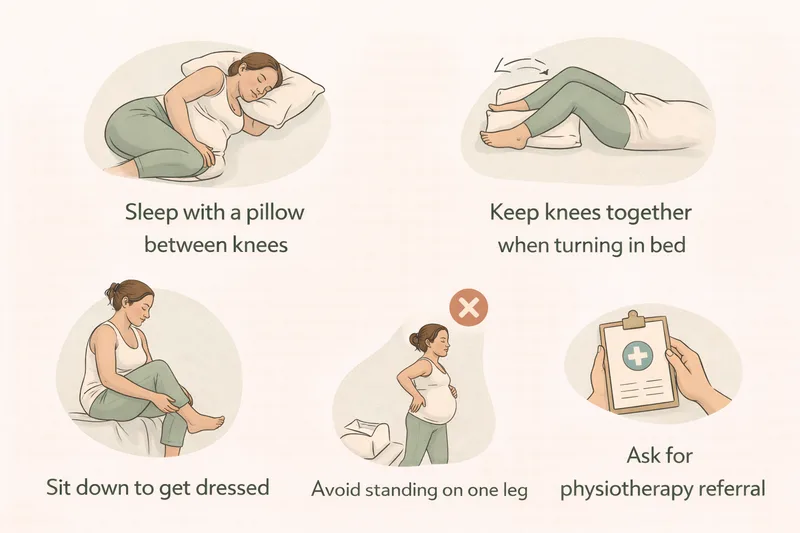
Sleep with a pillow between your knees. This helps keep your pelvis aligned and can reduce pain when turning in bed. Try to keep your knees together when turning over.
Sit down to get dressed. Avoid standing on one leg — for example when putting on trousers, socks, or shoes. Sit on the edge of the bed instead.
Take smaller steps. Shortening your stride can reduce the strain on your pelvis when walking.
Get in and out of the car carefully. Swing both legs out together rather than stepping out one leg at a time. A plastic bag on the seat can help you swivel more easily.
Avoid heavy lifting and carrying. This can worsen the strain on your pelvic joints.
Use stairs carefully. Go up one step at a time, leading with your least painful leg. Come down leading with the more painful side. If stairs are very painful, try going up and down on your bottom.
Pain relief. The NHS notes that paracetamol is generally considered safe in pregnancy. If you need stronger pain relief, speak to your GP.
Can You Still Have a Normal Birth?
Yes. According to the NHS, most women with PGP can have a vaginal birth. The key is planning ahead.
Write in your birth plan that you have PGP, so the people supporting you during labour and birth are aware. Your midwife or doctor should be able to work with you to find positions that are comfortable for labour and birth. Being in water can take the weight off your joints and allow you to move more easily, so a water birth may be worth discussing with your midwife.
The RCOG advises that if you have PGP, your midwife or doctor should be able to work with you to find comfortable positions for labour and birth.
Will It Go Away After Birth?
For most women, yes. According to Tommy's, the symptoms normally improve in the weeks or months after the baby is born, although around 1 in 10 people have symptoms for longer. The RCOG echoes this — PGP usually improves after birth, but if it persists, it is important to continue treatment.
If you are still experiencing pelvic pain a few weeks after birth and it is affecting your daily life, speak to your GP. You can be referred for postnatal physiotherapy, and continuing the exercises you were given during pregnancy can help your recovery.
The RCOG also notes that if you have had PGP in one pregnancy, you are more likely to have it again in a future pregnancy. Strengthening your abdominal and pelvic floor muscles before getting pregnant again can help reduce the risk.
The Mental Health Side
This is something that does not get talked about enough. Living with chronic pain during pregnancy — at a time when you are supposed to be "glowing" — can be deeply frustrating and isolating.
If PGP is affecting your mood, your confidence, or your ability to enjoy your pregnancy, that is a valid thing to raise with your midwife. You are not being dramatic. Pain that stops you from walking, sleeping, or looking after yourself is a real problem that deserves real support.
The Bottom Line
Pelvic girdle pain is common, it is not your fault, and it is not something you should just put up with. Treatment is available at any stage of pregnancy, and the earlier you ask for help, the better the outcome tends to be.
If you are limping, wincing when you turn over in bed, or dreading the stairs — tell your midwife. Ask for a physiotherapy referral. You do not need to wait until you cannot walk.
This article is for general information only and does not replace advice from your midwife, GP, or physiotherapist. If you are experiencing pelvic pain during pregnancy, speak to your maternity team — treatment is available and can help at any stage
This article was written in April 2026. We regularly review our content against the latest NHS and NICE guidelines to help ensure accuracy. This article references NHS: Pelvic Pain in Pregnancy, RCOG: Pelvic Girdle Pain and Pregnancy, and Tommy's: Pelvic Pain (SPD or PGP) in Pregnancy (reviewed December 2025). If you are experiencing pelvic pain during pregnancy, please speak to your midwife or GP — treatment is available and can help.



