It is 3am. You are exhausted. Your body is begging for sleep. But your bladder has other ideas. Your back aches. The baby is doing somersaults. And the moment you finally get comfortable, the heartburn kicks in.
Welcome to third trimester insomnia — one of the most common and least talked-about parts of late pregnancy. Everyone tells you to "sleep now while you still can," which is possibly the least helpful advice ever given to a pregnant woman who cannot actually sleep.
I remember being in tears at about 35 weeks because I had not had a proper night's sleep in what felt like weeks. I was exhausted during the day but wide awake at night. Nobody had warned me that this was normal — or that there were things that could help.
Quick answer: Sleep problems are very common in the third trimester and often get worse as pregnancy progresses. They are usually caused by physical discomfort, frequent urination, and anxiety. The NHS advises sleeping on your side after 28 weeks and offers practical tips for improving sleep.
How Common Is It?
Very common. A systematic review and meta-analysis in BMC Pregnancy and Childbirth found that the pooled prevalence of insomnia in the third trimester was 42.4%, although some individual studies reported much higher rates.
If you are lying awake right now reading this on your phone, you are in very large company.
Why Can't You Sleep?
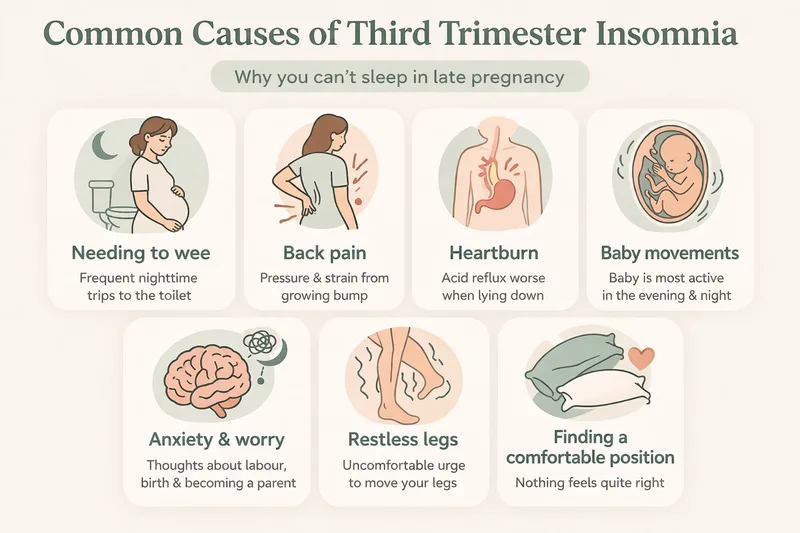
There is rarely one single reason. Third trimester insomnia is usually caused by a combination of physical, hormonal, and emotional factors piling up together.
You need to wee constantly. As your baby grows, the pressure on your bladder increases. Needing to get up two, three, or more times a night to use the toilet is one of the most common sleep disruptors in late pregnancy.
You cannot get comfortable. Finding a position that does not hurt your back, squash your bump, or make you feel like you are suffocating can feel impossible. As the bump gets bigger, the number of comfortable positions shrinks.
Heartburn. According to the NHS, heartburn is a common cause of sleep disruption in pregnancy. Hormonal changes relax the valve between your stomach and oesophagus, and the growing baby puts pressure on your stomach, pushing acid upwards — especially when you lie down.
Back pain and pelvic discomfort. Carrying extra weight puts strain on your lower back and pelvis, and many women find that lying down makes this worse rather than better.
Your baby is most active at night. Many women notice that their baby moves more in the evening and at night, just when they are trying to sleep. This is normal — but it does not make it any easier to drift off when you are being kicked from the inside.
Restless legs. Restless legs can also become a problem in pregnancy, especially later on. This uncomfortable, sometimes overwhelming urge to move your legs tends to be worst at night, just when you are trying to sleep. The exact cause is not fully understood, though it may be linked to iron levels.
Anxiety. As your due date approaches, worries about labour, birth, and becoming a parent can intensify. Lying in a quiet, dark room with nothing to distract you from your thoughts is exactly the environment where anxiety tends to get louder.
Hormonal changes. Rising levels of oestrogen and progesterone can disrupt your sleep cycle. The BMC Pregnancy and Childbirth review notes that sleep disturbances are common throughout pregnancy but intensify significantly in the third trimester, driven by a combination of hormonal, physical, and psychological factors.
The Safest Sleeping Position
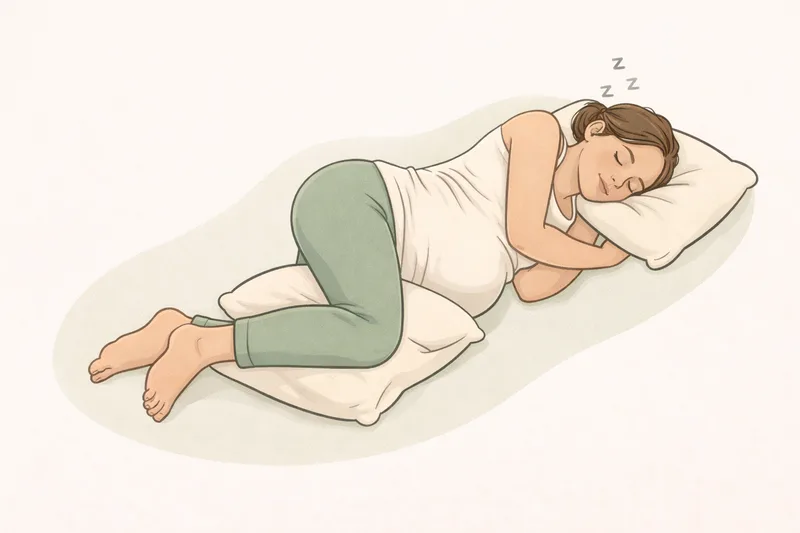
This is one area where the guidance is clear. The NHS advises that the safest position to go to sleep after 28 weeks is on your side — either left or right. Research suggests that falling asleep on your back after 28 weeks can double the risk of stillbirth, which may be related to the flow of blood and oxygen to the baby.
Tommy's echoes this advice and notes that it does not matter which side you go to sleep on — the research did not find a difference between left and right. The important thing is to start on your side.
If you wake up on your back, do not panic. The NHS is clear on this point: just roll back onto your side and go back to sleep. The risk relates to the position you fall asleep in, not brief moments during the night. Waking up on your back occasionally does not mean you have harmed your baby. This advice applies to daytime naps as well as night-time sleep.
Pillows can help. Try placing one between your knees to keep your hips aligned, and another under your bump for support. Many women find a full-length pregnancy pillow helpful, though a couple of ordinary pillows can work just as well.
What May Actually Help
There is no magic fix for third trimester insomnia, but there are practical things that can make a difference.
Limit fluids in the evening — but stay hydrated during the day. Reducing how much you drink in the hour or two before bed can help reduce overnight toilet trips without affecting your overall hydration.
Eat smaller meals in the evening. Large meals close to bedtime can worsen heartburn. The NHS suggests eating little and often rather than having one large evening meal. Avoiding spicy or greasy foods in the evening may also help.
Stay active during the day. According to the NHS, gentle exercise such as walking, swimming, or pregnancy yoga can help you feel less tired and may improve sleep quality. Try to avoid vigorous activity close to bedtime.
Cut caffeine from the afternoon onwards. The NHS advises avoiding tea, coffee, and cola in the evening, as caffeine can make it harder to fall asleep. During pregnancy, you should have no more than 200mg of caffeine per day.
Create a bedtime routine. A warm bath, gentle stretching, reading a book, or listening to a relaxation app can help signal to your body that it is time to wind down. The NHS suggests trying relaxation and breathing techniques, and avoiding screens before bed where possible.
Do not nap too late. If you need a daytime nap — and many women do — try to keep it earlier in the day. The NHS advises against napping in the afternoon or evening, as this can make it harder to fall asleep at night.
If you cannot sleep, do not lie there and fight it. Get up, do something quiet and low-stimulation — read, listen to a podcast, have a warm drink — and go back to bed when you feel sleepy. Lying in bed getting frustrated often makes insomnia worse, not better.
What About Sleep Aids and Medication?
This is an area where caution is needed. The BMC Pregnancy and Childbirth review highlights that sleep disorders in pregnancy are often overlooked and treated as a natural part of pregnancy, when in fact they can contribute to mental health problems and adverse outcomes if left unaddressed. However, any pharmacological treatment must be carefully weighed against possible risks to the baby.
Do not take any sleep medication — including herbal remedies and supplements — without speaking to your midwife or GP first. Some products that are considered safe outside of pregnancy may not be safe during it. This includes melatonin, valerian, and over-the-counter antihistamines marketed as sleep aids.
If your insomnia is severe and significantly affecting your daily functioning or mental health, speak to your GP. They may be able to offer support through NHS talking therapies, or in some cases, discuss medication options where the benefits clearly outweigh the risks.
When Should You Be Concerned?
Insomnia itself is not dangerous — the NHS notes that feeling tired will not harm you or your baby, although it can make daily life harder.
However, if your sleep problems are accompanied by persistent low mood, anxiety that feels overwhelming, or thoughts that worry you, it is important to tell your midwife or GP. The NHS notes that sleeplessness, when accompanied by other symptoms, can occasionally be a sign of depression, and support is available.
If you notice excessive snoring, pauses in breathing during sleep, or your partner tells you that you stop breathing at night, mention this to your midwife. In some cases, this may be a sign of obstructive sleep apnoea, which can develop or worsen during pregnancy and may benefit from assessment.
The Bottom Line
Third trimester insomnia is one of the most frustrating parts of late pregnancy. You are exhausted, you need sleep more than ever, and your body seems determined to make it as difficult as possible.
The good news is that it is temporary. It is not a sign that something is wrong. And while there is no cure, there are practical things you can do to improve your chances of getting some rest — even if "a full night's sleep" becomes "a few decent stretches."
Sleep on your side, keep your bedroom cool, and do not beat yourself up on the nights when sleep just does not come. Your body is doing something extraordinary. It is allowed to struggle with the basics while it does.
This article is for general information only and does not replace advice from your midwife, GP, or healthcare provider. If sleep problems are significantly affecting your daily life or your mental health, speak to your maternity team.
This article was written in April 2026. We regularly review our content against the latest NHS and NICE guidelines to help ensure accuracy. This article references NHS: Tiredness and Sleep Problems in Pregnancy, Tommy's: How Can I Get More Sleep in Pregnancy?, and Salari N et al. (2021). A systematic review and meta-analysis of prevalence of insomnia in the third trimester of pregnancy. BMC Pregnancy and Childbirth, 21, 284. If sleep problems are significantly affecting your daily life or mental health, please speak to your midwife or GP.



