Nobody warns you about the discharge. You'll hear about morning sickness, tiredness, and cravings — but nobody sits you down and says, "By the way, you're going to go through knickers like never before." It's one of those pregnancy symptoms that catches most women completely off guard, and because nobody talks about it openly, you end up googling at midnight wondering if something's wrong.
I remember mentioning it almost apologetically to my partner, like I thought something was off. It wasn't. It was completely normal — my body was doing exactly what it was supposed to do. But I didn't know that, because nobody had told me.
If that sounds familiar, this guide is for you. We'll walk through what's generally considered normal, what changes to expect at each stage of pregnancy, and — most importantly — the specific signs that mean you should pick up the phone and speak to your midwife.
Why Does Discharge Increase in Pregnancy?
During pregnancy, your body produces significantly more oestrogen and progesterone. These hormones increase blood flow to the pelvic area and stimulate the glands in the cervix to produce more mucus. This extra discharge — known medically as leucorrhoea — is generally understood to be your body's way of helping to keep the vaginal environment clean and reduce the risk of infections reaching the womb. A clinical review by Sim et al. (2020) in the Singapore Medical Journal notes that vaginal discharge can increase during higher oestrogen states such as pregnancy, and that healthy physiological discharge should not be associated with symptoms such as itching, redness, or a strong odour.
There's also a specific protective purpose. In early pregnancy, a thick plug of mucus forms in the cervix to help seal the opening of your womb. According to Tommy's, this mucus plug is thought to act as a barrier, helping to prevent bacteria from travelling up into the uterus where your baby is developing. It typically remains in place until your body starts preparing for labour in the final weeks.
NICE guideline NG201 advises that pregnant women should be informed that increased vaginal discharge is a common physiological change during pregnancy — though discharge accompanied by itching, soreness, an unpleasant smell, or pain on passing urine may suggest an infection that needs investigation.
So while it might feel uncomfortable or inconvenient, that extra discharge is generally a sign that your body's natural defence mechanisms are functioning as expected.
What Does Normal Pregnancy Discharge Tend to Look Like?
Normal pregnancy discharge typically shares a few consistent characteristics. It is usually clear to milky white in colour, with a thin or slightly watery consistency in early pregnancy that may become thicker as your pregnancy progresses. It generally has either no smell or a very mild one — not unpleasant or fishy — and according to the NHS, it should not cause itching, burning, or irritation.
The amount tends to increase throughout pregnancy, often becoming heaviest in the third trimester. Some women find they need to change their underwear more frequently than usual, especially towards the end. While this can feel like a lot, it is typically within the range of what's considered normal.
If your discharge broadly fits this description, it is unlikely to be a cause for concern. However, every woman's body is different, and what matters most is noticing changes from what is normal for you. If something feels different — even if you can't quite identify what has changed — that is always worth mentioning to your midwife.
How Discharge Changes Through Pregnancy

Discharge doesn't tend to stay the same from start to finish. Understanding the general pattern at each stage can help ease unnecessary worry.
First trimester: You may notice an increase in thin, clear or milky discharge quite early on. For some women, this can be one of the earliest signs of pregnancy — sometimes even before a missed period. This increase is generally driven by the surge of hormones that begins shortly after conception.
Second trimester: Discharge may become more noticeable and slightly thicker. It usually remains clear to white and should be mild-smelling or odourless. This is the stage where many women start using panty liners for comfort, which is fine as long as you choose unscented ones and change them regularly.
Third trimester: The volume may increase further. As you approach your due date, the NHS notes you may notice the discharge becoming heavier and possibly containing streaks of pink or blood-tinged mucus. This is often the mucus plug beginning to come away — sometimes called a "show" — and it can be a sign that your cervix is starting to prepare for labour. A show may happen days or even weeks before labour actually begins, so it does not necessarily mean things are imminent.
What Is the Mucus Plug?
Throughout pregnancy, a plug of thick mucus sits in the cervix, helping to seal the entrance to the womb. When your cervix begins to soften and dilate in the weeks or days before labour, this plug can come away — either all at once or gradually over several days.
The mucus plug typically looks like a blob of sticky, jelly-like discharge. It may be clear, yellowish, pinkish, or streaked with small amounts of blood. The NHS refers to this as a "show" and considers it a normal part of late pregnancy.
Losing your mucus plug does not necessarily mean labour is about to start. Some women lose theirs weeks before contractions begin. However, if you notice bright red blood rather than pink-tinged mucus, or if this happens before 37 weeks, contact your maternity unit for advice.
When Might Discharge Indicate a Problem?
While most pregnancy discharge is harmless, certain changes can sometimes indicate an infection or other complication that may benefit from treatment. NICE guideline NG201 recommends that healthcare professionals advise pregnant women that discharge accompanied by itching, soreness, an unpleasant smell, or pain when passing urine may point to an infection that needs to be investigated.
It's worth noting that most of these conditions are relatively common in pregnancy, are generally treatable, and when addressed promptly are not typically associated with serious harm. The key is recognising changes early and speaking to your midwife rather than waiting.
Green or yellow discharge with a strong or fishy smell may sometimes indicate bacterial vaginosis or, less commonly, a sexually transmitted infection such as trichomoniasis. These can often be treated with antibiotics or other medication. A review by Rao and Mahmood (2020) in Obstetrics, Gynaecology & Reproductive Medicine notes that trichomoniasis infection in pregnancy may be associated with an increased incidence of preterm birth and low birth weight, though outcomes vary. If you notice this type of discharge, contact your midwife or GP. NICE recommends that a vaginal swab may be considered for pregnant women with symptomatic vaginal discharge if there is any doubt about the cause.
Thick, white, cottage cheese-like discharge with itching or soreness may suggest thrush (vaginal candidiasis). According to the NHS, thrush is thought to be more common during pregnancy because hormonal changes can alter the vaginal environment and make it easier for yeast to overgrow. Sim et al. (2020) note that an estimated 10–20% of women of reproductive age may carry Candida, with colonisation rates thought to increase during pregnancy. Thrush is not generally considered harmful to a developing baby, but it can be very uncomfortable.
For treatment, NICE recommends vaginal imidazole — such as clotrimazole or econazole — for vaginal candidiasis during pregnancy. The NHS advises speaking to your midwife or doctor before using any thrush treatments while pregnant, as some products commonly used outside of pregnancy are not recommended during it.
Watery discharge that feels like a continuous trickle or a sudden gush — particularly before 37 weeks — may indicate that your waters have broken early. According to Tommy's, this is called preterm prelabour rupture of membranes (PPROM), and it is generally considered to require prompt medical attention because it may increase the risk of infection and could lead to preterm labour.
It can sometimes be difficult to distinguish between a heavy increase in normal discharge and leaking amniotic fluid. A practical way to check: if you put on a clean maternity pad and find it noticeably damp within an hour or so — and this continues — it may be more likely to be amniotic fluid than discharge. Normal discharge tends to be intermittent, whereas leaking waters often feels like a slow, steady trickle that you cannot control. If you're unsure, it is always worth contacting your maternity unit. They would rather check and reassure you than have you worrying at home — and a simple assessment can usually help determine the cause.
Vaginal bleeding at any stage of pregnancy should be discussed with your midwife or maternity unit. While light spotting can sometimes occur without a concerning underlying cause, persistent or heavy bleeding generally needs prompt assessment. NICE recommends that unexplained vaginal bleeding after 13 weeks be reviewed in secondary care.
A noticeable change in smell, even without an obvious colour change, is worth raising with your midwife at your next appointment. Changes in odour can sometimes be an early indicator of an infection developing.
When Should You Contact Your Midwife?
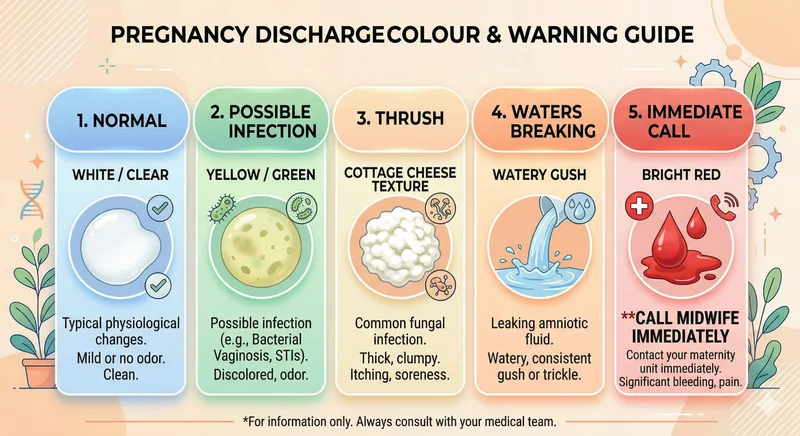
Consider contacting your midwife, GP, or maternity unit if you notice any of the following: a change in the colour of your discharge to green, yellow, or grey; a strong, fishy, or unpleasant smell; itching, burning, or soreness around the vagina or vulva; watery discharge that leaks continuously or comes as a sudden gush; any vaginal bleeding — particularly before 37 weeks; or if something simply doesn't feel right to you.
Trust your instincts. Your midwife would far rather hear from you and put your mind at ease than have you sit at home worrying. Discharge-related concerns are among the most commonly raised topics at antenatal appointments, and there is nothing embarrassing about asking.
If you experience a sudden gush of fluid or any heavy bleeding, do not wait for your next appointment — contact your maternity unit or delivery suite immediately.
Practical Tips for Managing Discharge in Pregnancy
There are some simple things that may help you stay comfortable and support your vaginal health during pregnancy:
Use unscented panty liners if the volume of discharge is bothersome, and change them regularly throughout the day. Scented liners may cause irritation for some women.
Wear cotton underwear where possible, as cotton tends to be more breathable than synthetic fabrics and may help maintain a healthier environment.
Wipe from front to back after using the toilet, to help reduce the risk of transferring bacteria from the bowel to the vagina.
Wash your vulva with plain water or a mild, unscented soap. The NHS advises that the vagina cleans itself naturally and does not need douching, vaginal washes, or perfumed products. These can disrupt the natural balance of bacteria and may actually increase the risk of infection.
Do not use tampons during pregnancy. Panty liners are generally considered fine, but inserting anything into the vagina during pregnancy could potentially introduce bacteria.
The Bottom Line
Increased discharge during pregnancy is one of those things that nobody talks about but nearly every pregnant woman experiences. In most cases, it is considered completely normal — your body is simply working to help protect you and your baby from infection.
The key is knowing what's typical for you and being aware of the specific changes that should prompt a conversation with your midwife. Clear or milky white, mild-smelling, no itching or soreness — that is generally reassuring. Anything that's an unusual colour, has a strong or unpleasant smell, causes discomfort, or feels like leaking fluid — speak to your midwife.
It's not glamorous. It's definitely not the part of pregnancy you'll see on anyone's Instagram. But it's normal, it's protective, and it's absolutely nothing to be embarrassed about.
This article is for general information only and does not replace advice from your midwife, GP, or healthcare provider. If you have any concerns about changes in vaginal discharge during pregnancy, always contact your maternity team.
This article was written in April 2026. We regularly review our content against the latest NHS and NICE guidelines to help ensure accuracy. This article references NICE guideline NG201: Antenatal Care (published August 2021, last reviewed December 2024), NHS: Vaginal Discharge in Pregnancy (last reviewed April 2024), Tommy's: Vaginal Discharge During Pregnancy, Sim M, Logan S, Goh LH (2020). Vaginal discharge: evaluation and management in primary care. Singapore Medical Journal, 61(6), 297–301, and Rao VL, Mahmood T (2020). Vaginal discharge. Obstetrics, Gynaecology & Reproductive Medicine, 30(1), 11–18. If you have any concerns about your health during pregnancy, please speak to your midwife, GP, or maternity unit.



